A 34-year-old man with an 8-year history of outbreaks of oral and genital ulcers presented with high fever and skin lesions that had developed 21 days earlier, without abdominal pain. Computed tomography revealed intestinal perforation requiring surgery. After treatment with corticosteroids and azathioprine proved to be ineffective, it was switched to adalimumab.
Paciente de sexo masculino de 34 años con antecedente de úlceras orales y genitales que cursaban en brotes de 8 años de evolución, se presenta con fiebre elevada y lesiones en piel durante 21 días, sin dolor abdominal. Se realiza tomografía computarizada, observándose perforación intestinal, por lo que es intervenido quirúrgicamente. Es tratado con corticoides y azatioprina. Luego, por falta de respuesta, se le administra adalimumab.
Behçet's disease (BD) is a chronic multisystemic inflammatory disease characterized by outbreaks of vascular involvement in some lesions, but not in others that affect brain parenchyma or in pseudoacne. Thus, whether it should be considered a vasculitis is a matter of debate.
Case ReportThe patient was a 34-year-old Caucasian who had been hospitalized with a syndrome that had begun 21 days earlier. It consisted of high fever of unknown origin, together with weakness and a nodular eruption that left scars in both upper and lower limbs, and no ophthalmologic manifestations.
He reported an 8-year history of intermittent painless oral and genital ulcers that appeared and disappeared spontaneously, with no definite diagnosis.
Laboratory tests showed: erythrocyte sedimentation rate >120mm/h, C-reactive protein 400mg/dL and negative results on immunological tests (antiphospholipid antibodies, antineutrophil cytoplasmic antibodies, anticardiolipin antibodies and the venereal disease research laboratory test). Antigen tests, viral serology and a test for human leukocyte antigen (HLA)-B27 were negative. An electrophoretic protein profile was normal. Immunoglobulin (Ig) A level was 443mg/dL. Parasitological analysis of stool was negative.
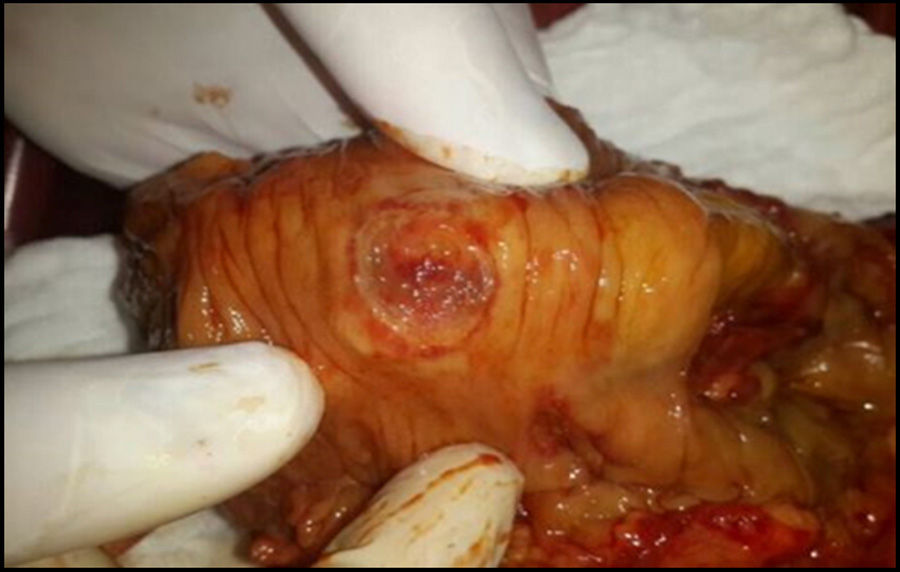
Thoracic and abdominal computed tomography revealed bilateral pleural effusion, pneumoperitoneum, peritoneal membrane thickening, free fluid in the peritoneal cavity and enlarged lymph nodes. Therefore, he was scheduled for surgery, and was found to have numerous intestinal perforations (Fig. 1). It was necessary to perform subtotal colectomy and ileostomy. Treatment with meprednisone at 40mg/day resulted in a favorable clinical course. The dose was reduced to 8mg/day, accompanied by azathioprine at 100mg/day, which resulted in 1 year without relapses. A video recording of a follow-up colonoscopy showed active lesions, and he began to receive 40mg of subcutaneous adalimumab every 15 days,1–3 which achieved clinical and histopathological remission after 4 months of treatment.4
Ancillary histopathological studies of a tissue specimen demonstrated colonic ulceration with perilesional inflammation; a skin biopsy revealed septal lobular panniculitis with mononuclear and polymorphonuclear cell infiltrate; and nonspecific inflammation was observed in the scrotal ulcer. Testing was positive for HLA-B525 and negative for HLA-B51. The pathergy test was negative.
ConclusionsPatients with Behçet's disease can experience oral and genital ulcers for years, with no definitive diagnosis, and consult their physicians only when serious complications arise. Since the diagnosis is mainly clinical, primary care physicians should be familiar with the characteristics of this disease,6 especially in countries like Argentina in which the prevalence is low and the evidence is concealed in a variety of symptoms that must be associated to discovery it. Therefore any delay in the diagnosis increases the rates of mortality and morbidity affecting patients with BD.
To date, when gastrointestinal involvement is detected, good responses have been achieved with sulfasalazine, azathioprine and corticosteroids at low or high doses or as pulse therapy, as well as with pulse cyclophosphamide. However, in the case of intestinal perforation, the treatment must be aggressive and can be initiated directly with adalimumab.7
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of InterestThe authors declare they have no conflicts of interest.
Please cite this article as: Della Maggiora M, Baños A, Paolini V, Florio D, Takashima L, Aicardi P. Enfermedad de Behçet con perforación intestinal: a propósito de un caso. Reumatol Clin. 2017;13:171–172.