Leishmaniasis is a parasitic disease caused by the intracellular protozoa Leishmania. It is transmitted by through the bite of a mosquito: the female phlebotomus. There are 21 species of Leishmania. The species most widespread in Spain is Leishmania infantum and its major reservoir is the dog.1
A number of cases of leishmaniasis have been reported in patients with different rheumatic diseases who were being treated with biological drugs.
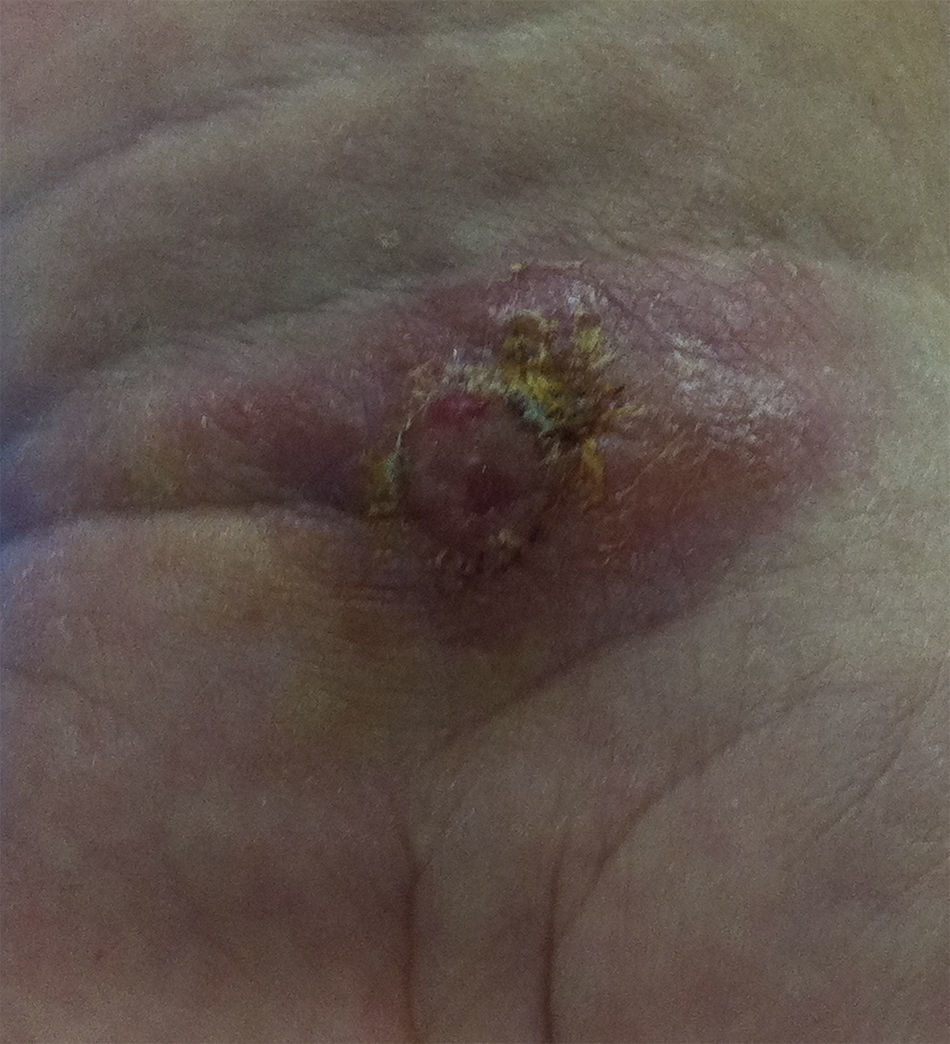
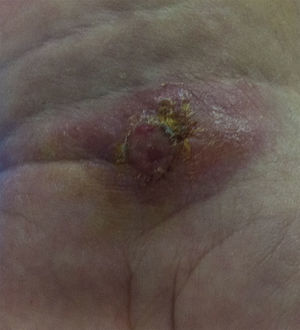
We describe a case of cutaneous leishmaniasis in a woman with rheumatoid arthritis who was receiving an anti-tumor necrosis factor (TNF)-α and methotrexate. The patient was 54 years old and had been born in Murcia, a city in southeastern Spain. She had been diagnosed with rheumatoid arthritis 5 years earlier, and was positive for rheumatoid factor and anti-cyclic citrullinated peptide antibodies. She was being treated with subcutaneous methotrexate (25mg each week) together with adalimumab at a dose of 40mg every 15 days. She had no significant medical history or harmful habits. The patient was in clinical remission and it was decided to increase the interval between adalimumab doses to 21 days. Weeks later, she developed a nodular and ulcerated lesion on the palmar side of her left carpus (Fig. 1). Biopsy led to a diagnosis of cutaneous leishmaniasis. Immunosuppressive therapy was discontinued and she underwent an analytical and imaging study, which ruled out visceral leishmaniasis. The patient was treated with amphotericin B at a dose of 3mg/kg body weight/day for 5 days, and the lesion disappeared. Intralesional treatment was not performed and there were no secondary effects of the therapy.
In Spain, according to a report of the Ministry of Health dated 2012, the autonomous communities that had reported cases of leishmaniasis during the preceding decade were: Andalusia, Aragon, Balearic Islands, Cantabria, Castile-León, Catalonia, Valencian Community, Extremadura, Community of Madrid, Region of Murcia, Chartered Community of Navarre and La Rioja. According to the registry of the Center for the Coordination of Health Warnings and Emergencies, between 2002 and 2010, 82 cases were reported in Murcia.
The disease can present in 3 clinical forms2: cutaneous, mucocutaneous and visceral leishmaniasis. In the cutaneous and mucocutaneous forms, the diagnosis is reached by biopsy and visualization of Leishmania in the cells.
The mucocutaneous form presents with erythema, erosion and ulcers around the lips and nose; the differential diagnosis should include Wegener granulomatosis, among others. In the cutaneous form, we find lesions in areas of exposed skin, like face, arms and legs. Each lesion represents a bite. Visceral leishmaniasis can present with a febrile syndrome with constitutional symptoms and manifestations depending on the affected organs (spleen, liver, bone marrow, among others).2
Tumor necrosis factor-α is a cytokine implicated in the immune response against intracellular parasites. It has been involved in granuloma formation and in containing the protozoa.3
Since the introduction of anti-TNF-α agents, there have been several cases of leishmaniasis.4 According to the reports, it seems that the risk is greatest during the first year of treatment, and to a greater extent with infliximab than with the subcutaneous drugs.5,6 There have also been cases with other types of immunosuppressive agents, like azathioprine, methotrexate, cyclosporine, steroid and cyclophosphamide.7
In immunocompromised patients, the risk of reactivation, and thus, of active visceral leishmaniasis is increasing.4,7 In regions in which it is endemic, in an immunocompromised patient with fever, asthenia, splenomegaly and pancytopenia, this diagnostic possibility should be considered.4 In our case, the patient was receiving treatment with an immunosuppressive agent, and came from an area in which leishmaniasis is endemic. Thus, upon the first diagnostic suspicion, after the development of the skin lesion, the latter was biopsied and immunosuppressive therapy was discontinued.
Please cite this article as: Moreno Martínez MJ, Moreno Ramos MJ, Sánchez Pedreño P. Leishmaniasis cutánea. Una infección oportunista. Reumatol Clin. 2017;13:181–182.