Behçet's disease (BD) is a rare autoimmune disease, with distinctive features like recurrent oral ulcers and, in most cases, genital ulcers. The symptoms can also include ophthalmological, neurological, dermatological, vascular, musculoskeletal, intestinal and pulmonary manifestations.1 Involvement of the larynx is not common. We report the case of an individual with BD that affected a vocal cord.
The patient was a 58-year-old man who had stopped smoking 3 years earlier and had no other medical history of interest. He came to the department of internal medicine with recurrent oral and genital ulcers that had developed 2 months earlier. They were accompanied by fever and he felt generally unwell. Moreover, he also had a 2-week history of dysphonia, with no other associated symptoms.
Physical examination revealed dysphonia and the presence of painful scrotal and oral ulcers. In addition, he had an acneiform eruption on his back and lesions compatible with erythema nodosum on lower limbs. He presented no other problems.
Laboratory analyses disclosed leukocytosis, neutrophilia and an elevation of acute-phase reactants: 14,000leukocytes/mm3 (78% neutrophils) and a C-reactive protein level of 150mg/L.
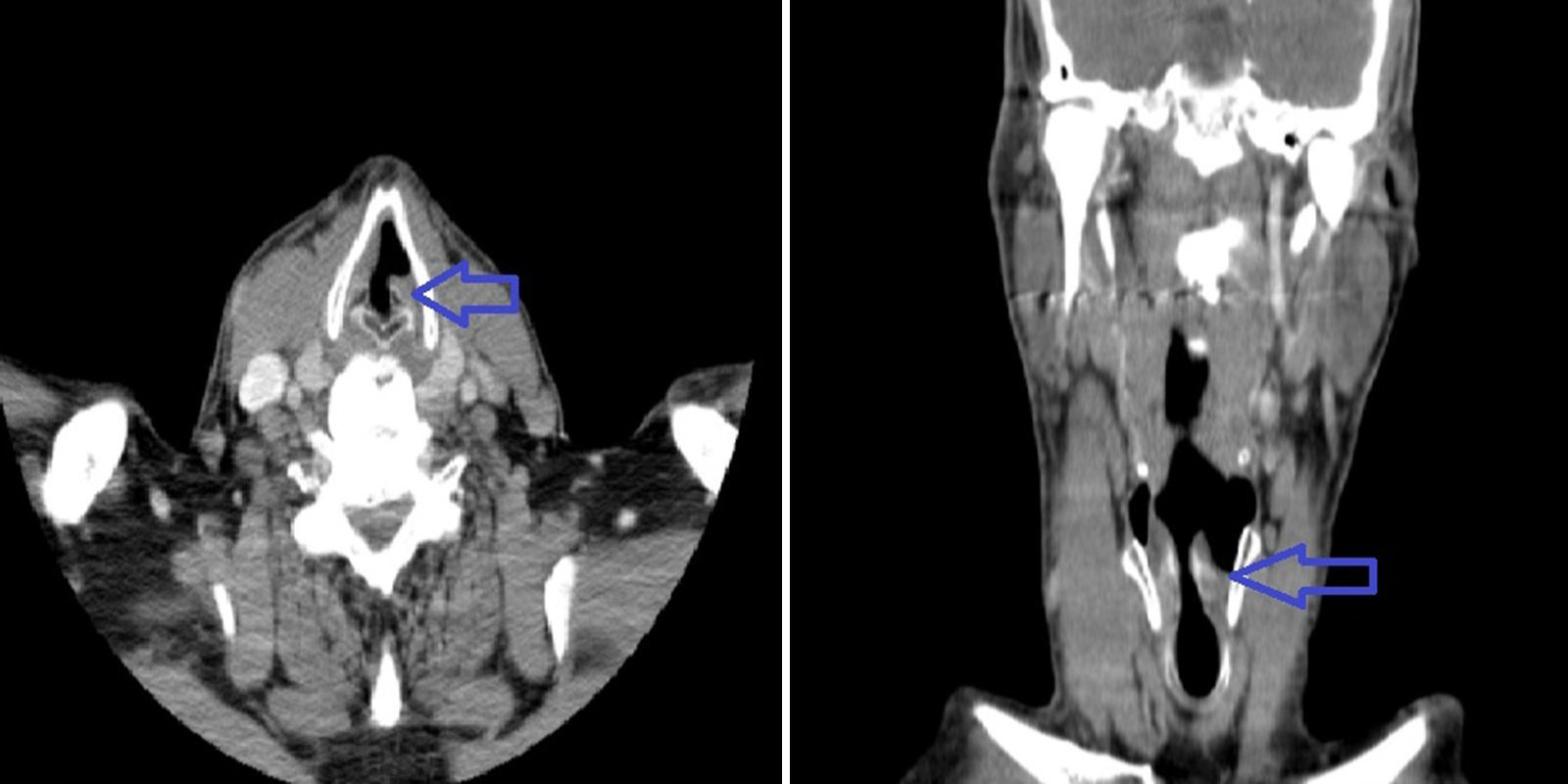
Cranial computed tomography (CT) showed no evidence of ischemic or hemorrhagic cerebral vascular involvement. Cervicothoracic CT (Fig. 1) revealed paralysis of left vocal cord, whereas abdominal CT disclosed infrarenal abdominal aortic aneurysm measuring 47mm×48mm, with no other findings.
The study of ear, nose and throat confirmed paralysis of left vocal cord. There was no ophthalmological involvement. Tests for autoimmunity included antinuclear antibodies, antineutrophil cytoplasmic antibodies, antiphospholipid antibodies, rheumatoid factor and anti-cyclic citrullinated peptide antibodies, all negative. Serological tests ruled out bacterial infectious diseases like syphilis, Lyme disease and chlamydiosis and polymerase chain reaction for herpesvirus 1 and 2 and cytomegalovirus was negative. Blood cultures were also negative.
The patient underwent a pathergy test in right arm, which was positive, and a punch biopsy of the skin in the region of the acneiform eruption on his back showed evidence only of pseudofolliculitis. Given the clinical suspicion of BD, treatment was begun with oral glucocorticoids at a dose of 20mg a day. The treatment with corticosteroids improved the ulcers and skin lesions, but there was no change in the dysphonia. The aneurysm observed in CT images subsequently required surgical treatment, which was successful.
Behçet's disease is an immune-mediated systemic vasculitis, characterized by the presence of recurrent orogenital ulcers, ocular inflammation and skin lesions. The etiology and pathogenesis of BD are unknown, although it has been demonstrated that the presence of human leukocyte antigen (HLA) B51 constitutes an important genetic predisposing factor, especially among patients from the Middle and Far East.1
Being a multisystemic vasculitis, almost any part of the organism can be affected. The oral ulcers, recurrent and painful, are present in 90%–100% of the patients with BD. Other frequent clinical manifestations are genital ulcers (60%–80%), ocular lesions (67%–95%), skin lesions (41%–94%), arthritis (47%–69%) and neurological involvement (8%–31%).2 The cutaneous manifestations of the patient we describe was nearly diagnostic of BD.
In contrast to central nervous system involvement, which is common in BD, peripheral nervous system manifestations are rare. There have been isolated cases of Guillain–Barré syndrome, mononeuritis multiplex, sensorimotor neuropathy, autonomic neuropathies and subclinical nerve conduction abnormalities.3 However, vocal cord involvement is unusual and, to date, only 2 cases have been reported in the medical literature.4,5
The most probable explanation for this occurrence could be the presence of vasculitis at the level of the recurrent laryngeal nerve.5 In the case of this patient we found no other condition to explain the dysphonia.
In conclusion, BD should be taken into account in the differential diagnosis of sudden dysphonia in the absence of other more common findings, especially in regions in which the disease is frequent.
Please cite this article as: Amao-Ruiz E, Correa-Fernández AM, Gallego-Gil J. Parálisis de cuerda vocal como manifestación clínica de enfermedad de Behçet. Reumatol Clin. 2017;13:306–307.