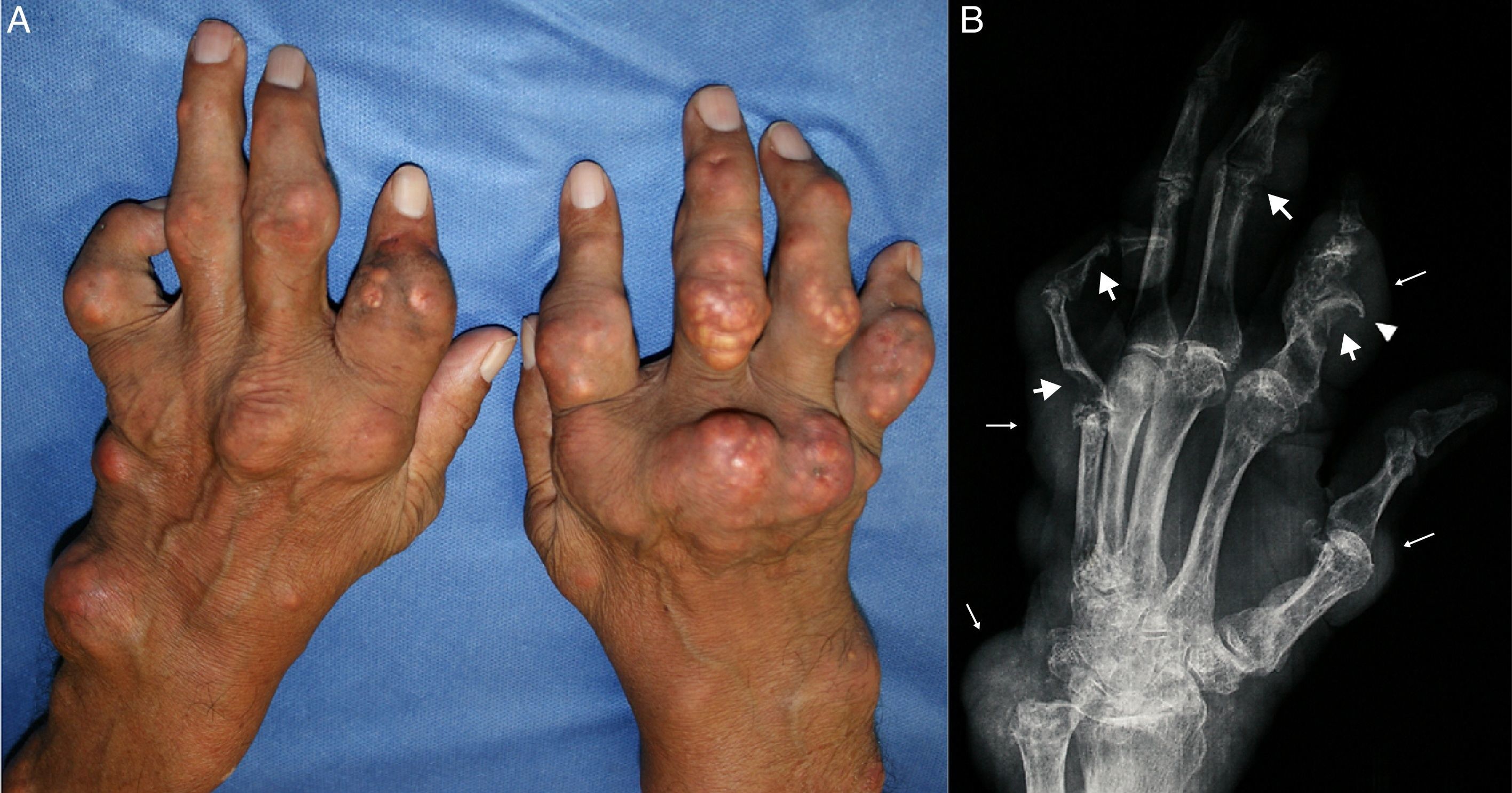
The patient is a 60-year old man we attended during a rheumatology campaign at his hometown, Etzatlan, Mexico. He has a 30-year history of gout and presented widespread tophus formation with extensive structural damage (Fig. 1). Based on the model of health determinants described by the WHO,1 we depict the failures that explain why a supposedly easy-to-treat disease2 progressed to polyarticular chronic tophaceous gout with multidimensional impact.
Genes predispose to the disease but do not determine outcomes. Regarding education and individual lifestyle, the patient had 2 years of schooling, frequently drank alcohol, and had a strong internal locus of control. Regarding healthcare services, the patient attended over 25 general practitioners (GPs), receiving different prescriptions and several contradictory indications, mainly on how to take allopurinol which varied from daily suboptimal doses to periodic use as “prophylaxis” when the patient planned to drink alcohol. The patient visited a rheumatologist once, who explained the disease in detail and how to treat it. But the patient did not understand and the rheumatologist did not make sure he understood. In fact, the patient perceived great disagreement among the visited physicians, so he decided what to do: take bethametasone, limit alcohol intake to weekends, and assigned allopurinol as the cause of worsening because every time he took it had an acute attack. Community and social networks also failed. He always attended medical appointments alone; his wife and children are resentful because he has not worked for the last 15 years and his children had to start working, which prevented them from attending high school. The socioeconomic and cultural conditions, such as myths surrounding the disease, the use of nonconventional therapies, and living in a small town without specialized medical services also had a negative impact.
Unfavorable health determinants may explain the reported increase in severity of gout in several countries3–7; there are several protagonists involved on these. In the sense of shared responsibility, the poor outcome of this patient, and of many others as reported in the literature, can be assigned not only to the patient's behavior, but also to GPs and their misconceptions; the inefficiency of social and community networks; the rheumatologist and his unadjusted communication skills towards his patient's culture; the health-care system and its inability to care for people beyond the activities of diagnosing and prescribing drugs to just the ones that attend to the clinics, etc. Perhaps if only one of the protagonists had done his job well, such multidimensional impact of an “easy-to-treat disease” would not have occurred.
FundingNone.
Conflict of interestThe authors declare that they have no conflict of interest.
None.