Calcium pyrophosphate deposition disease is a common arthropathy characterised by the articular or periarticular deposit of microcrystals of dehydrated calcium pyrophosphate.1,2 Clinical presentation is highly variable, including no symptoms to joint symptoms with different patterns of involvement, which may mimic other diseases such as rheumatoid arthritis or septic arthritis.3 As a result, this entity should frequently be taken into account in many differential diagnoses in rheumatology.
Clinical caseA 77-year-old woman was admitted to hospital to assess a 2 week onset of fever of 38°C mainly in the evening, without any clear clinical signs, combined with shivering and sweating, asthenia and anorexia. Physical examination in the emergency department revealed no relevant findings. The only remarkable history of interest was that the patient referred to swelling, pain and functional impotence of her left ankle, with no trauma involved, 3 weeks earlier. She had presented at another hospital and had been diagnosed with a probable sprain and had received treatment with NSAIDS, rest and cold presses with an improvement of symptoms as a result.
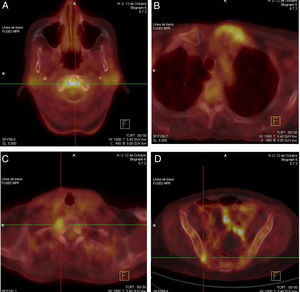
During hospitalisation a broad analytical study was conducted, which included tumour markers and autoimmunity which only showed up a microcytic hypochromic anaemia with Hb 9.9g/dL (subsequently dropping to 7.8g/dL) with no other changes in the haemogram and a raised CRP level of 5.7mg/dL. An extensive microbiological study involving several blood cultures, urine culture, multiple serologies (HIV, hepatotropos virus, CMV, VEB, parvovirus B19, lues, Mycoplasma, Brucella, Borrelia, Leishmania), Mantoux and IGRA reasonably ruled out the presence of infection. A chest X-ray, echocardiogram, gastroscopy and colonoscopy, gynaecological ultrasound and bone marrow biopsy were also requested, the results of which were normal. Finally a PET-CAT was performed where the only findings of interest was a marked increase in the metabolism in the left sternoclavicular, right sacroiliac, right costovertebral of T1 and atlantoaxial joints (Fig. 1), suggestive of inflammatory polyarticular disease.
At this time interconsultation was made with the rheumatology service which requested plain X-rays as part of the study of the hands and knees which showed chondrocalcinosis in the triangular fibrocartilages of the carpus and meniscus femorotibial joints. An ultrasound study was made, where hyperchoic images were found, suggestive of calcium pyrophosphate deposit crystals in the thickness of the bilateral femoral cartilage, mild to moderate synovial leakage in the right knee and mild leakage in the left tibio-astragaline joint. Arthrocentesis of the right knee produced synovial fluid with inflammatory characteristics and the presence of calcium pyrophosphate crystals under optical microscope examination.
As infectious and tumour aetiologies had been reasonably ruled out and considering the microcrystalline disease as the most probable cause of the symptoms, we decided to initiate treatment with a 1mg/day dose of colchicine, with the fever disappearing for the first time in almost 3 weeks in hospital and normalisation of CRP. The patient was therefore discharged. The patient has not presented with fever in any of the successive check-ups, the anaemia has improved and no further symptoms have presented.
DiscussionCalcium pyrophosphate deposition disease may present clinically in highly variable ways. In the case we describe, the patient presented with constitutional and febrile syndromes with no medical focus and with inflammatory data from analysis (elevated CRP and chronic anaemia), but was found to be asymptomatic from an articular viewpoint save for the history of probable acute left ankle monoarthritis which had presented previously. The joint involvement revealed in the PET-CAT at atlantoaxial, sternoclavicular, costovertebral and sacroiliac joint level (all of them reported in the disease, from pyrophosphate deposition and also frequently subclinical as in this case4,5) guided diagnosis, with the microcrystal deposit showing up in the X-rays and ultrasound6,7 and essentially through analysis of the synovial fluid, which guided treatment enabling the patient's symptoms to be resolved.
Although several case series have been described in the literature with fever, constitutional syndrome and marked raising of acute phase reactants as the principal form of disease presentation by calcium pyrophosphate deposition,8–10 with initially absent joint manifestations or unremarkable symptoms, we have not found any studies in which the percentage of patients with this atypical presentation form have been assessed. It is important to be familiar with and evoke this entity to avoid costly, invasive procedures and unnecessary treatments.
Conflict of interestsThe authors have no conflict of interests to declare.
Please cite this article as: Lozano Morillo F, de la Cámara Fernández I, Rabadán Rubio E. Síndrome constitucional y fiebre prolongada en relación con enfermedad por depósito de pirofosfato cálcico de presentación atípica. Reumatol Clin. 2020;16:366–367.