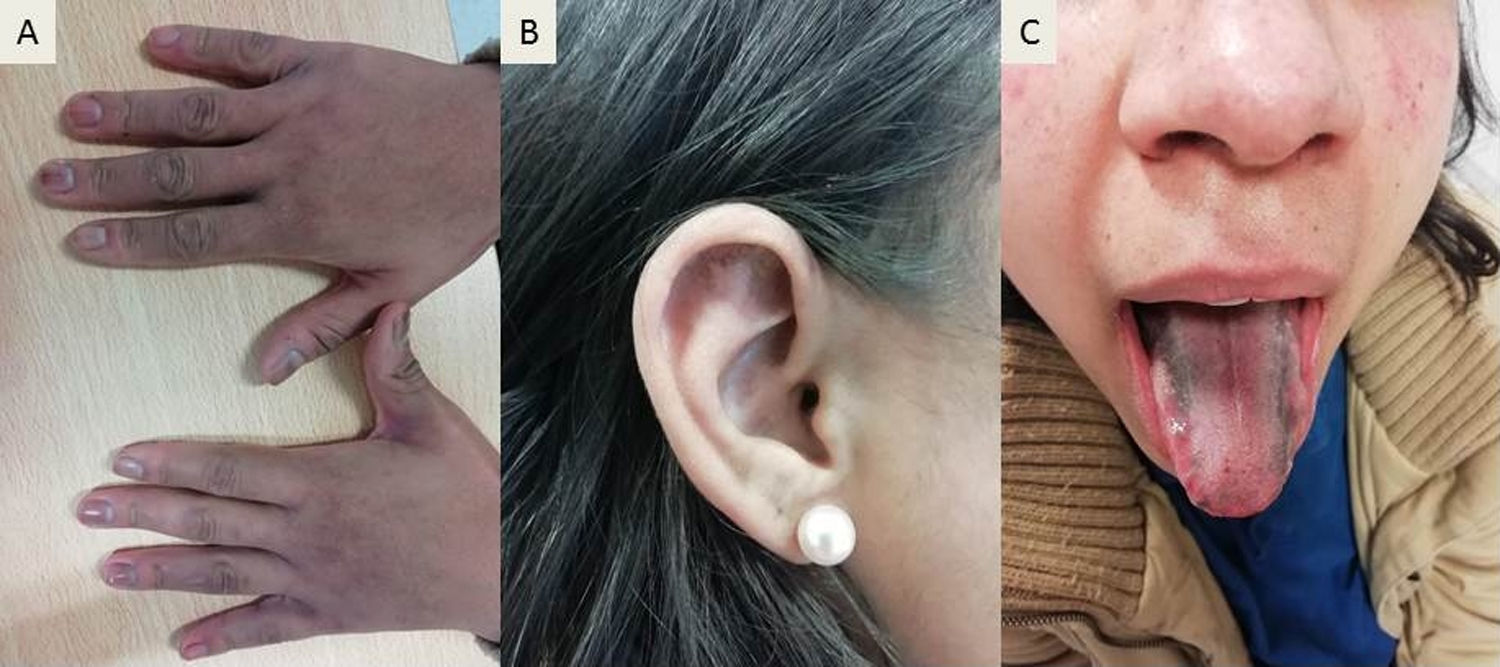
A 29-year-old Brazilian woman with a previous diagnosis of Systemic Lupus Erythematosus with articular, cutaneous, serous and hematological involvement who immigrated to Portugal 7 months prior presented to our rheumatology department for continuation of care. She was chronically medicated with hydroxychloroquine 400mg for the past 10 years as well as prednisolone 10mg and levothyroxine 88mcg. The objective examination showed hyperpigmentation of the nails of the hands (Fig. 1 – Panel A), the scapha and triangular fossa of the ears (Fig. 1 – Panel B) and the tongue (Fig. 1 – Panel C) that was suggestive of hydroxychloroquine induced hyperpigmentation. Other causes of pigmentary changes such as endocrine or metabolic disorders as well as other drug-induced pigmentation were excluded. An ophthalmologic evaluation with OCT was performed and retinopathy was excluded.
Hydroxychloroquine induced hyperpigmentation is an underreported adverse event that may appear in about 10–25% of the patients after long-term use.1–3 It appears mainly on the anterior side of the legs but can also affect other less reported areas such as the nail bed, head, and mucosa.1,2,4 The pathogenesis of this adverse event is poorly understood.2,3 It is important to consider that hydroxychloroquine induced hyperpigmentation may mimic other pigmented conditions, namely melasma, Addison's disease, hemochromatosis, Wilson's disease and vitamins deficiencies.5 It usually improves after drug discontinuation.5
Informed consentInformed consent has been obtained from the patient.
FundingThis research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflict of interestNone.