Hemangioblastomas are uncommon lesions that represent nearly 4% of the tumors of the spinal cord. Three fourths of them are sporadic, and the remainder are components of von Hippel Lindau (VHL) disease.1,2 They are mostly found in the cerebellum, although they can develop in the brain stem or spinal cord; of the latter, they are only rarely located in the filum terminale.3 The filum terminale is a delicate thread-like portion of fibrous tissue, a modification of the pia mater. It is about 20cm long and originates at the vertex of the conus medullaris at the base of the coccyx, providing longitudinal support to the spinal cord.
Case ReportWe present the case of a woman who, at the time of the diagnosis, was 70 years of age and had a history of hemithyroidectomy for a thyroid nodule, as well as acromegaly due to a growth hormone and prolactin-producing pituitary adenoma. This lesion was removed using a transsphenoidal approach and her postoperative healing was satisfactory. She also had osteopenia and osteoarthritis of both knees, with total replacement of right knee.
She came to the rheumatology department for the first time after a history of several months of low back pain that was progressively more disabling, and was treated with radiation of both lower limbs. Maneuvers to evaluate radicular pain were negative and there was no motor or sensory deficit; however, the patient experienced paresthesia.
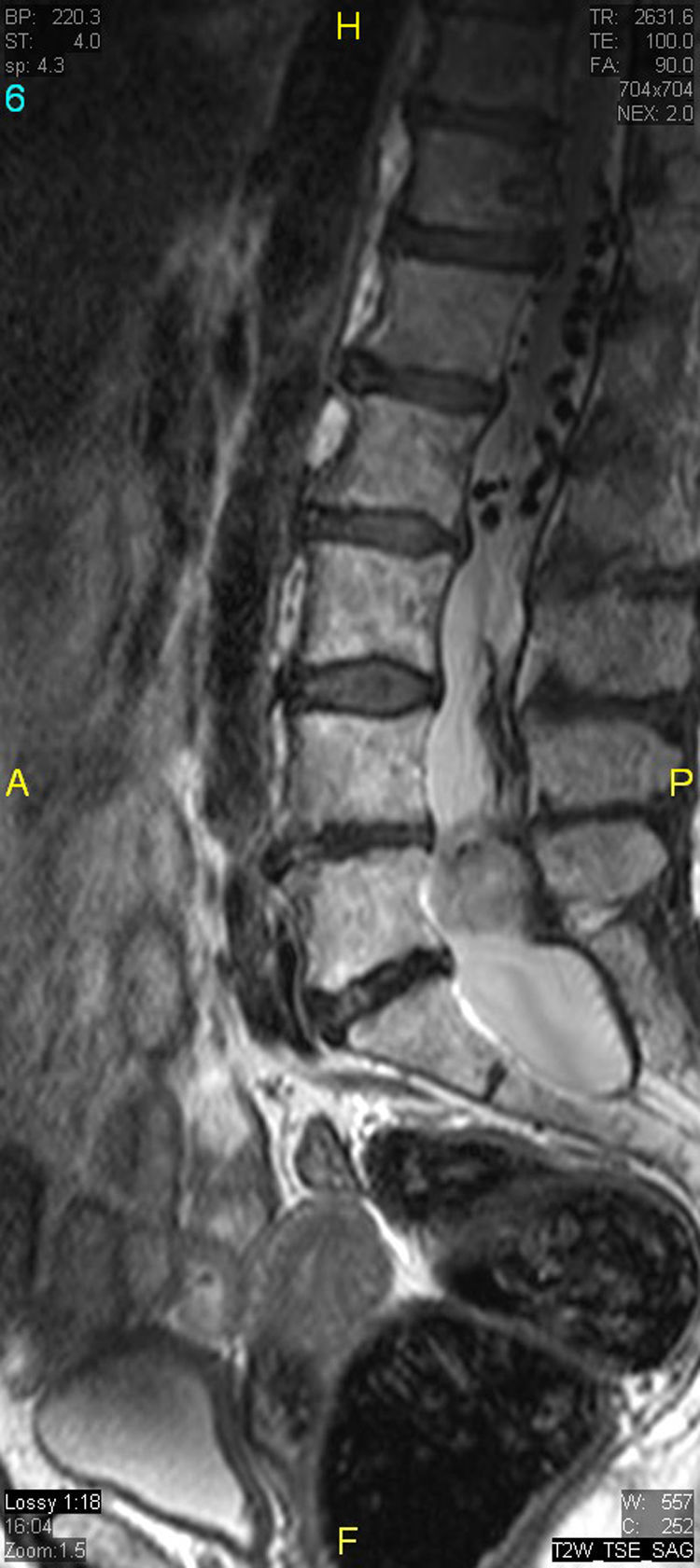
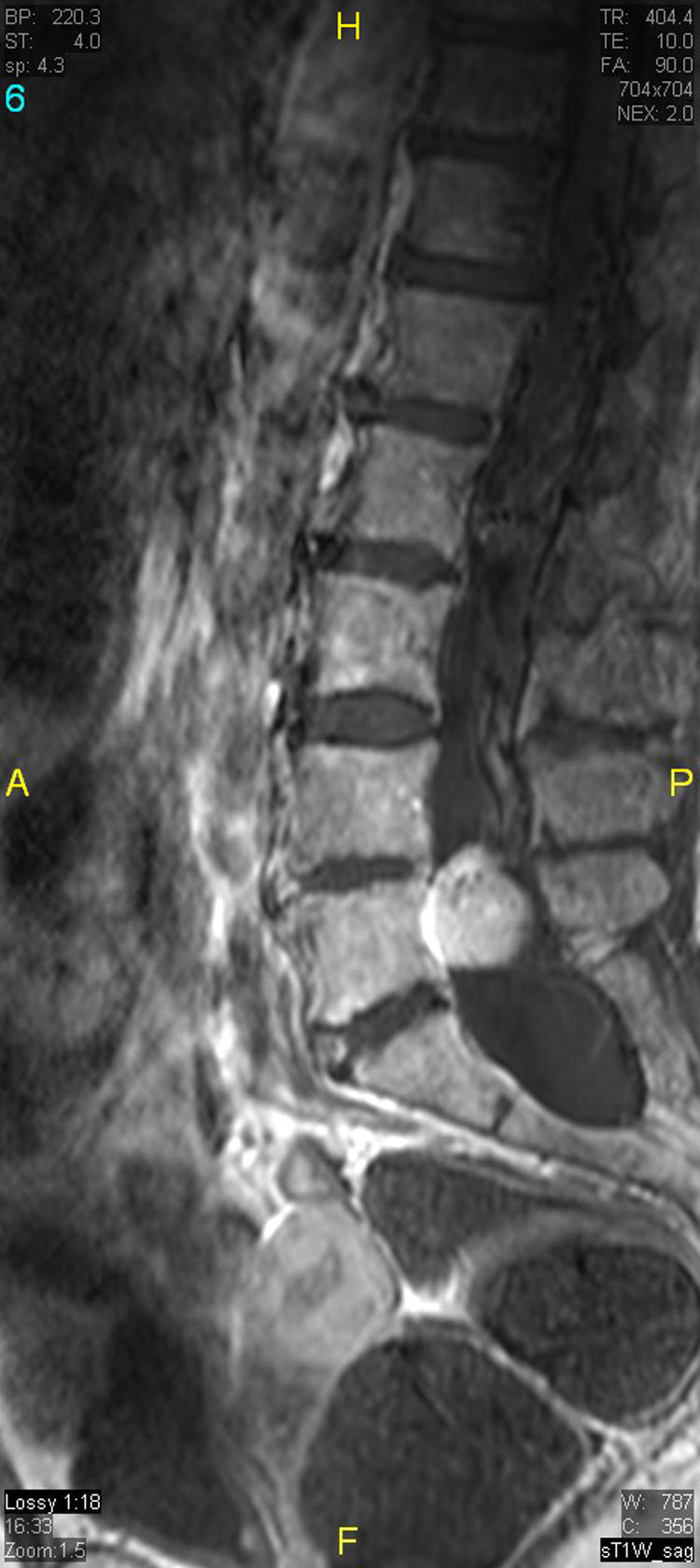
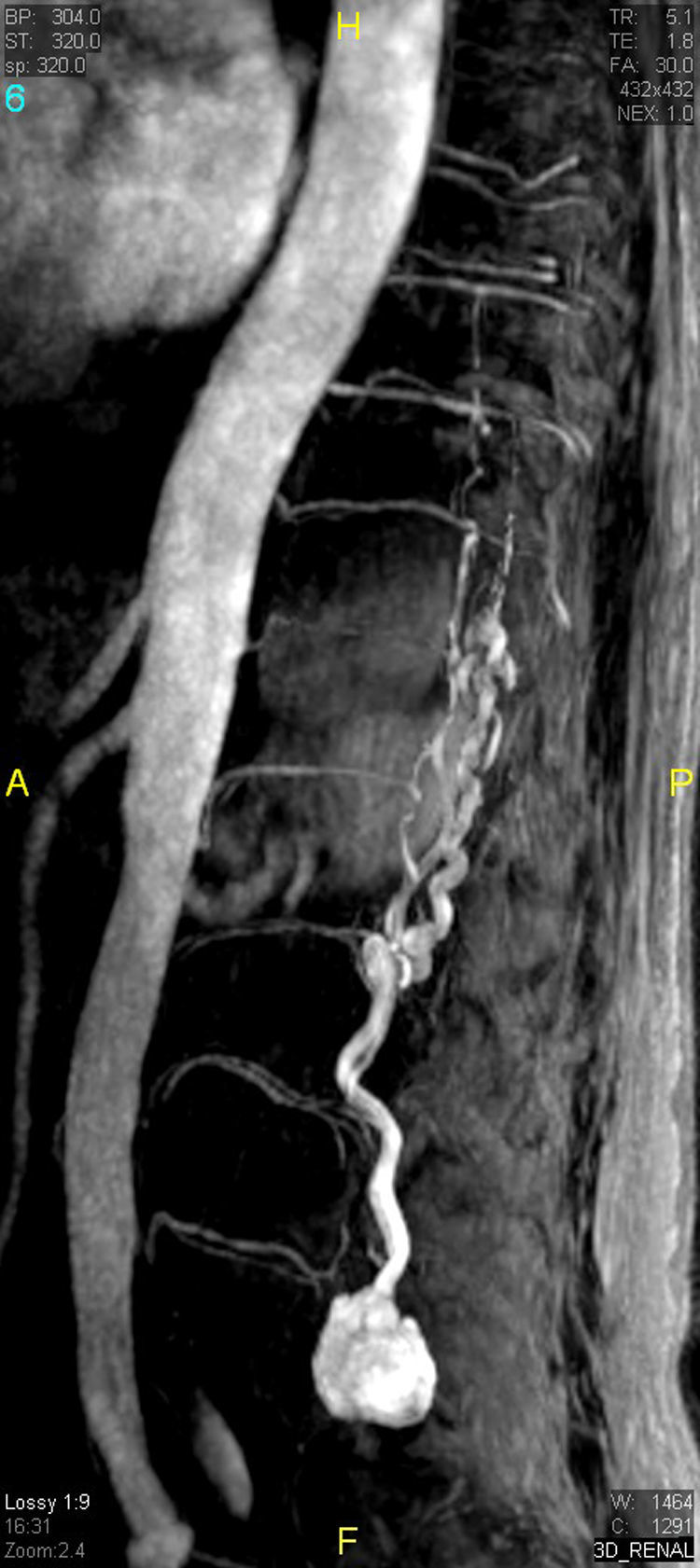
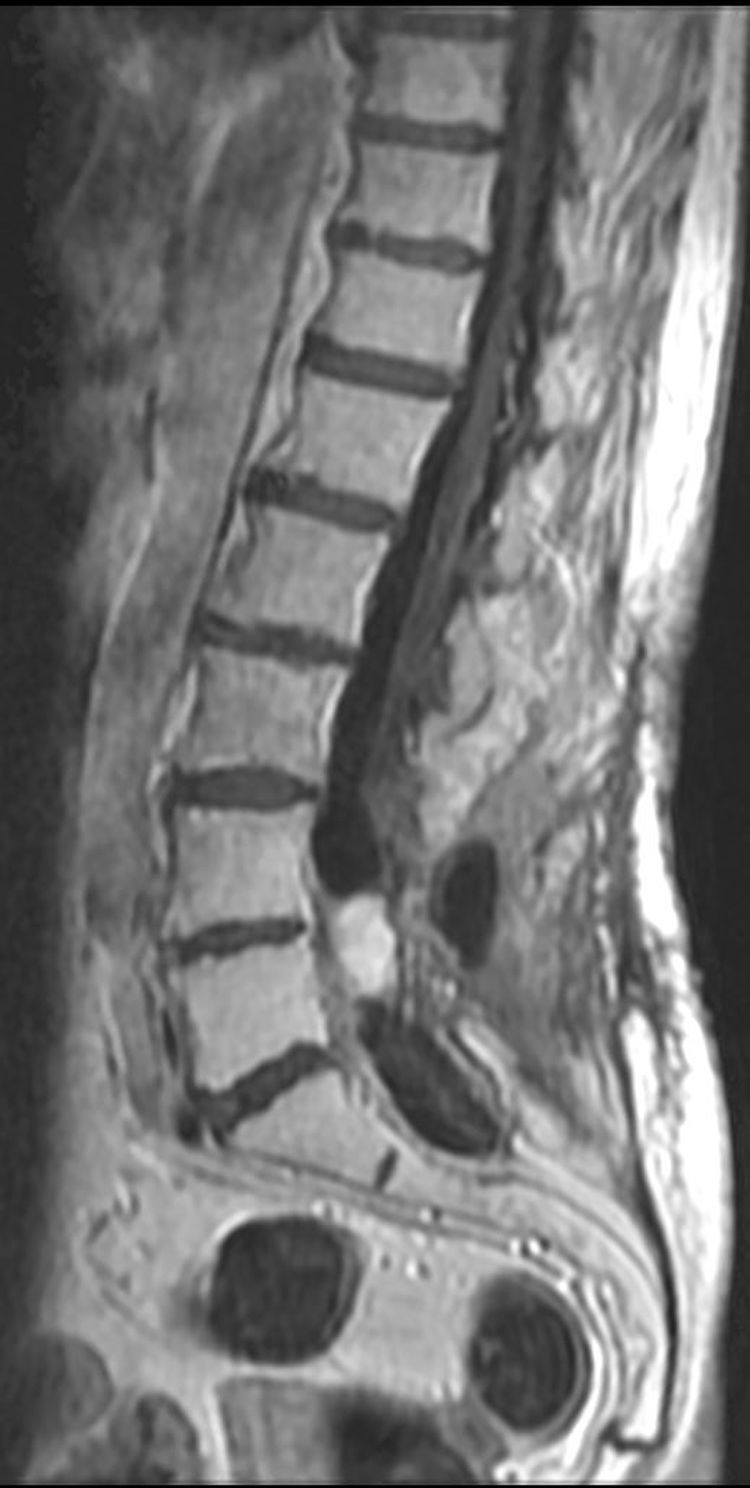
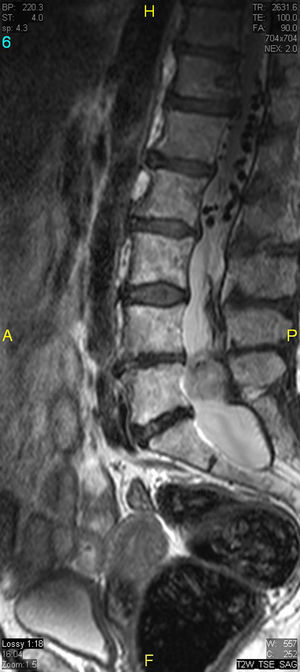
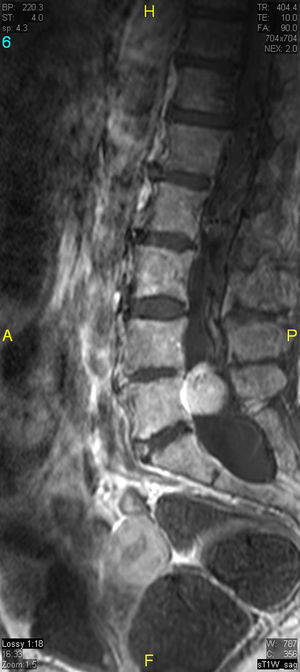
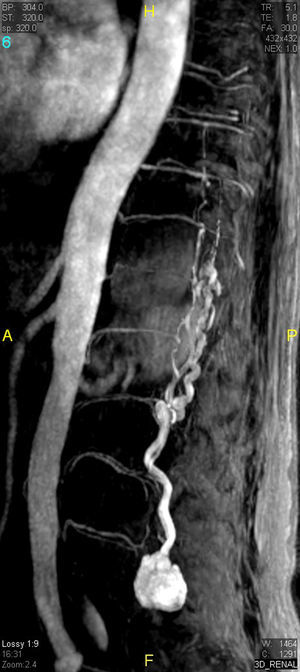
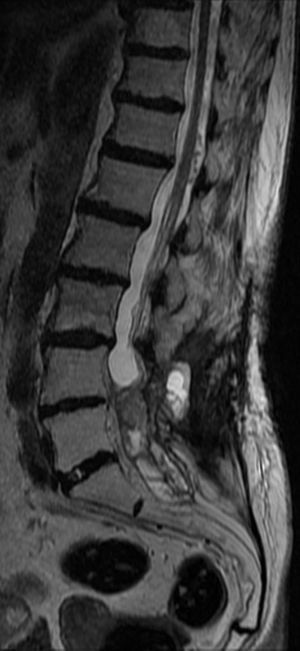
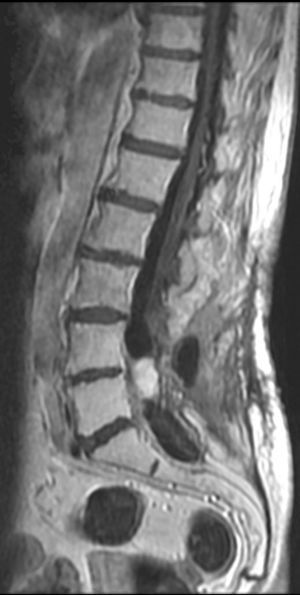
The patient underwent magnetic resonance imaging (MRI) of the low back, which revealed an intradural space-occupying lesion in the conus medullaris. It was hypervascularized and receiving its supply of blood from a rosary-like vessel,4 that extended from T10, occupying nearly the entire spinal canal to the level of L5. Spinal angiography confirmed the presence of a hypervascularized tumor irrigated by a medium-sized artery and a large, tortuous anterior spinal artery that was not amenable to embolization5,6 (Figs. 1–3).
Contrast-enhanced magnetic resonance angiographic image. Sagittal plane with maximum intensity projection reconstruction. The image shows the mass, as well as the dilated vascular structures. Because of the static nature of the examination, the view does not show the origin of the blood supply.
Given that the tumor could progress and result in subsequent clinical deterioration, we explained the therapeutic possibilities to the patient, and the decision was made to intervene surgically.7
In the operating room, we observed a red mass totally adhered to the roots of the filum terminale. Clips were placed both on the artery and the vein. There was no marked modification in the size or the bleeding of the mass. Under intraoperative neurophysiological monitoring, the resection was highly complex because of the constant tendency of the mass to bleed8 and its adherence to the nerve roots. We resected only 90% of the tumor because of the lability of the roots that were most closely in contact with the lesion. As a postoperative neurological sequela, the patient developed certain urinary incontinence, but the low back pain that radiated to her extremities had disappeared. Biopsy confirmed the diagnosis of hemangioblastoma; the study of the extension of the disease ruled out the existence of other hemangioblastomas.
The patient remained asymptomatic until the fourth year of follow-up, when she experienced a recurrence, with lumbosciatic pain in her right leg, and lumbosacral MRI revealed tumor progression. Because of the neurological risk of further surgery, the decision was made to embolize the lesion via right pedicle of L4, which resulted in its marked devascularization. After the procedure, the patient remained asymptomatic until the clinical signs reappeared 3 months later. Magnetic resonance imaging showed that the lesion continued to progress, and the decision was made to reoperate. This procedure achieved very limited resection due to adherence of the tumor and scar tissue to the L5 and S1 nerve roots, making it necessary to interrupt the intervention due to the risk of significant neurological sequelae.
After the failure of the surgical approach, it was decided to initiate focal radiotherapy9,10 with 54Gy over 27 sessions. The patient showed a good clinical response and there was a reduction in the size of the tumor.
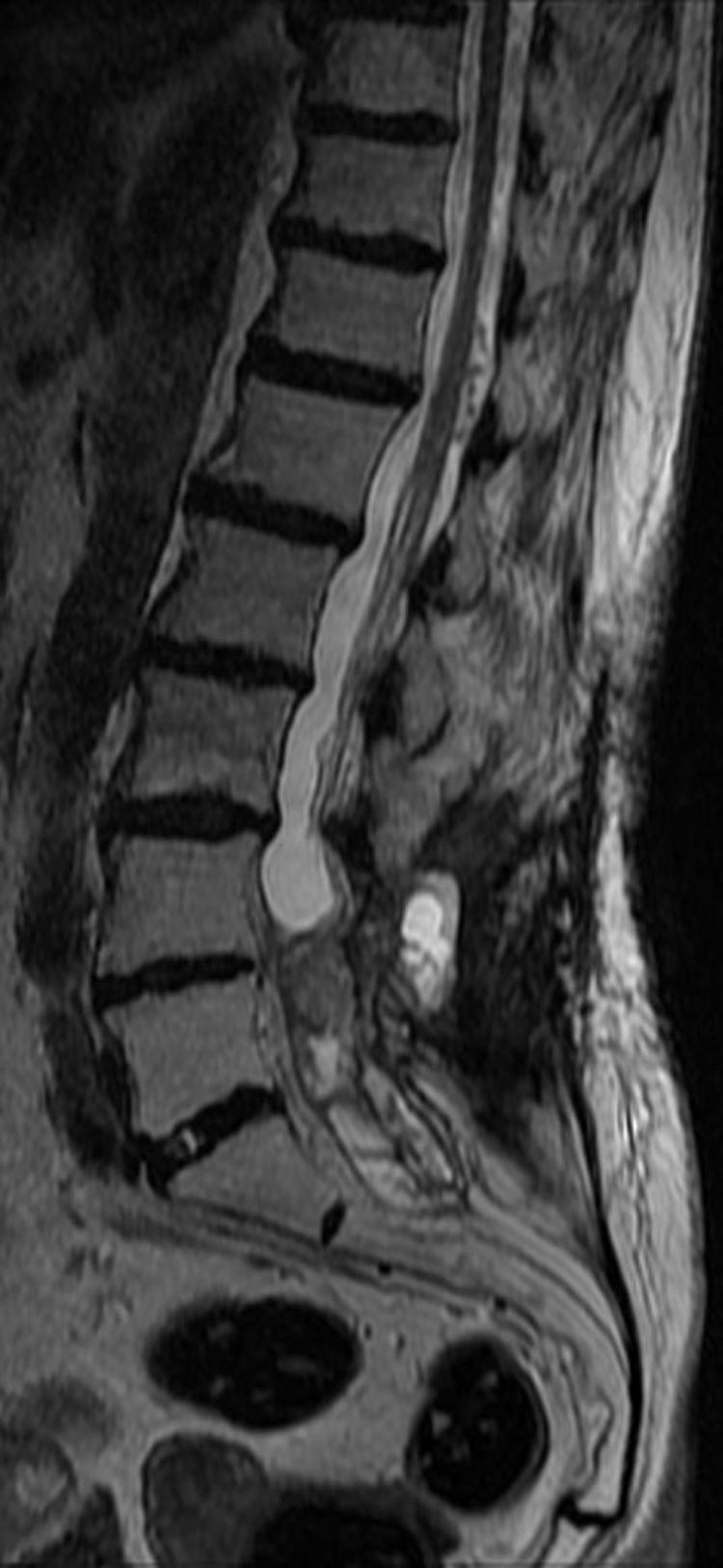
To date, she continues to undergo clinical monitoring every 6 months and annual radiological evaluation, and is asymptomatic and the lesion has not grown (Figs. 4 and 5).
Hemangioblastomas are slow-growing tumors. Sporadic lesions are usually solitary and are often in regions associated with greater neurological compromise; they typically affect young men (40 years) and are rare both in older persons and in children. In individuals with VHL disease, the usual age at the time of diagnosis is approximately 29 years.
The clinical manifestations are those derived from the location of the space-occupying lesion. The treatment of these patients should be chosen with this in mind due to the potential sequelae that can result from a surgical intervention at the site of the tumor; surgery should be an option reserved for those individuals who are symptomatic.
Although it is true that the lesions can often be completely removed, it must be taken into account that the recurrence rate ranges between 16% and 30% and that of operative mortality from 8% to 15%, whereas the 5-year survival is 90%.
In this case, the sequelae of urinary incontinence had been discussed and was acceptable to the patient, who had scaled the entire analgesic ladder in the unsuccessful attempt to treat her severe low back pain.
Both surgical management and that based on radiation have a role, and must be selected in accordance with the characteristics of the lesion and the patient, although there are no randomized clinical trials that compare or determine the time demanded by the different therapeutic actions. There is increasing evidence that supports the role of stereotaxic surgery and radiotherapy in selected patients with multiple tumors and those of difficult surgical access and in postoperative recurrence.
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that they have followed the protocols of their work center on the publication of patient data.
Right to privacy and informed consentThe authors declare that no patient data appear in this article.
Conflicts of InterestThe authors declare they have no conflicts of interest.
Please cite this article as: Salman-Monte TC, Castro-Dominguez F, Villalba G, Capellades J, Monfort J. Ciatalgia de presentación atípica en paciente con hemangioblastoma de filum terminale. Reumatol Clin. 2018;14:115–118.