Temporal arteritis (TA) is the most common form of systemic vasculitis. Its diagnosis is based on criteria proposed by the American College of Rheumatology (1990), and its treatment is high-dose corticosteroids.
Our objective is to assess the cost of diagnosing TA, and secondarily, cost-effective analysis of different diagnostic strategies (clinical, biopsy, doppler ultrasound) and therapeutic strategies (corticosteroid suspension).
Material and methodObservational, retrospective study has been carried out on patients with AT (2012–2021). Demographic data, comorbidities, signs and symptoms suggestive of AT were collected. AT was diagnosed with a score ≥ 3 according to American College of Rheumatoloy criteria (ACR-SCORE). The costs of diagnosis and treatment modification were analysed.
ResultsSeventy-five patients have been included, median age 77 (46–87) years. Headache, temporal pain and jaw claudication were significant for the diagnosis of TA.
Patients with a halo on Doppler ultrasound and a positive biopsy have significantly elevated ESR and CRP compared to patients who do not.
The cost of the AT diagnosis was 414.7 euros/patient. If we use ACR-SCORE ≥ 3-echodoppler it is 167.2 є/patient (savings 59.6%) and ACR-SCORE ≥ 3-biopsy 339.75 є/patient (savings 18%). If the corticosteroid was removed and a biopsy was performed, 21.6 є/patient (94.7% savings), if the corticosteroid was removed and Doppler ultrasound was performed, 10.6 є/patient (97.4% savings).
ConclusionsHeadache, temporary pain and jaw claudication are predictors of AT. Elevated ESR and CRP are predictors of positive biopsy and presence of halo on ultrasound.
The uses of ACR-SCORE ≥ 3 with Doppler ultrasound or biopsy, and with corticosteroid suspension, are cost-effective.
La arteritis de la temporal (AT) es la forma más frecuente de vasculitis sistémica, su diagnóstico está basado en criterios propuestos por el Colegio Americano de Reumatología (1990) y su tratamiento son corticoides a dosis elevadas.
Nuestro objetivo es valorar el gasto del diagnóstico de la AT, y secundariamente análisis coste-efectivo de distintas estrategias diagnósticas (clínica, biopsia, ecodoppler) y terapéuticas (suspensión del corticoide).
Material y métodoEstudio observacional, retrospectivo de pacientes con AT (2012–2021). Se recogieron datos demográficos, comorbilidades, signos y síntomas sugestivos de AT. Se diagnosticó AT con una puntuación ≥ 3 según criterios del American College of Reumatology (ACR-SCORE). Se analizaron los gastos del diagnóstico y modificación de tratamiento.
ResultadosSetenta y cinco pacientes, mediana edad 77 (6–87) años. Cefalea, dolor temporal y claudicación mandibular fueron significativos para el diagnóstico de AT.
Los pacientes con halo en ecodoppler y biopsia positiva, presentaron elevación de VSG y PCR de forma significativa en comparación con los pacientes que no.
El gasto diagnóstico de AT fue de 414,7 є/paciente. Si empleamos ACR-SCORE ≥ 3-eco-Doppler serían 167,2 є/paciente (ahorro del 59,6%) y ACR-SCORE ≥ 3-biopsia 339,75 є/paciente (ahorro del 18%). Si se retiraba corticoide y se realizaba biopsia hubiesen sido 21,6 є/paciente (ahorro del 94,7%), si se retiraba corticoide y se realizaba eco-Doppler hubiesen sido 10,6 є/paciente (ahorro del 97,4%).
ConclusionesCefalea, dolor temporal y claudicación mandibular son predictores de AT. La elevación de VSG y PCR son predictores de biopsia positiva y presencia de halo en ecografía.
El empleo de ACR-SCORE ≥ 3 con ecodoppler o con biopsia, y con suspensión del corticoide son coste-efectivos.
Temporal artery arteritis (TA), also known as cranial arteritis or Horton's arteritis, belongs to the family of giant cell arteritis, which are granulomatous vasculitides affecting medium and large calibre arteries. It occurs mainly in individuals over 50 years of age, with a peak incidence in the eighth decade. It is more prevalent in females (3:1).1,2 The incidence in Spain is around 10 cases per 100,000 population.3
Diagnosis is based on the criteria proposed in 1990 by the American College of Rheumatology (ACR-SCORE),4 which include clinical signs and symptoms typical of the disease: age >50 years, localised headache of recent onset, pain on palpation of the temporal artery or decreased pulse, sedimentation rate >50 mm/hour in the first hour, histological abnormalities (necrotising arteritis or granulomatous process with multinucleated giant cells). The presence of 3 or more of the 5 parameters establishes a diagnosis of TA with a sensitivity of 93.5% and a specificity of 91.2%.4
TA biopsy is usually performed on an outpatient basis with a surgical time of 20−50 min. It has a complication rate of between .5% and 1%; the main complication is bleeding (haemorrhage or haematoma), followed by surgical wound infection, nerve damage, vascular damage (arterial or venous), skin necrosis, or stroke. We did not assess complications associated with biopsy in this study, because we currently use minimally invasive techniques and biopsy is an invasive procedure.5 Biopsy remains the gold standard for the diagnosis of TA.2
Treatment with high-dose glucocorticoids is indicated for these patients, which have many side effects such as bone fractures, avascular necrosis of the hip, diabetes mellitus, infections, gastrointestinal bleeding, cataracts, and hypertension.2,6
Cost-effectiveness analyses are not used to find the cheapest or most effective technique, but to optimise health system resources to achieve the maximum health benefit with the available resources.7,8
In our hospital, TA is diagnosed by the internal medicine department, which requests the analyses, ultrasound, and biopsies. The aim of this study is to determine the costs generated by this diagnosis and, secondly, to conduct a cost-effectiveness study of different diagnostic strategies (clinical, biopsy, and/or Doppler ultrasound) and treatment (whether a negative diagnosis of TA implies discontinuation of corticosteroids).
Material and methodWe conducted a single-centre, retrospective observational study, according to clinical practice, of patients with suspected TA from 2012−2021. Patients with a primary and secondary diagnosis of temporal artery arteritis were requested from the hospital coding service. Approval for this study was obtained from the hospital’s ethics committee (PI 21-2443).
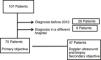
Population included in the study and descriptive analysis of the variablesPatients with a diagnosis of TA made in our hospital after 2012. In this period there were 107 patients with a diagnosis of TA, of which 32 patients were excluded (26 diagnosed before 2012, 6 diagnosed in a different hospital) (Fig. 1).
Demographic data and comorbidities were collected, as well as signs and symptoms suggestive of TA, analytical data such as ESR > 20.00 mm and CRP > 5.00 mg/dl, Doppler ultrasound assessing for the presence of halo sign, and biopsy with the presence of multinucleated giant cells. A diagnosis of TA was considered with an ACR-SCORE greater than or equal to 3.
Economic studyThe costs generated by temporal artery biopsy and Doppler ultrasound were analysed, as published in the Official Gazette of Castilla y León (BOCYL),9 where biopsy costs ;339.75 and arterial Doppler ;167.26.
The Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement (CHEERS) was used as a guide.10
Statistical analysisSPSS® 18 and G-Stat 2.0 statistical software were used for statistical analysis of the sample variables. Contingency tables were used to compare categorical variables, using Fisher's exact test or the χ2 test whenever possible; the ANOVA test was used for quantitative variables. A P-value of <.05 was considered statistically significant. To analyse the validity of Doppler ultrasound and of biopsy, sensitivity and specificity were calculated by comparing with the diagnosis according to an ACR-SCORE ≥ 3; corticosteroid discontinuation or modification of treatment was also established as an impact criterion.
ResultsPopulation included in the study and descriptive analysis of the variables: Table 1General characteristicsFor the primary objective, 75 patients with a median age of 77 years (46–87) were included; 41 (54.7%) were women.
Histories included 46 cases with HT (61.3%), 20 cases with dyslipidaemia (26.7%), 15 cases with diabetes mellitus (20%), 11 cases with COPD (14.7%), one case with renal failure (1.3%), 21 cases with polymyalgia rheumatica (28%), and 22 cases with heart disease (29.3%). None of the histories were statistically significant for diagnosis of TA, Table 1.
Characteristics of the patients diagnosed with temporal arteritis.
| Percentage | P-value | ||
|---|---|---|---|
| Median age | 77 years | ||
| Male | 34 | 45.3 | .315 |
| Female | 41 | 54.7 | .315 |
| History | cases | ||
|---|---|---|---|
| HT | 46 | 61.3 | .437 |
| Heart disease | 22 | 29.3 | .761 |
| Polymyalgia rheumatica | 21 | 28 | .635 |
| Dyslipidaemia | 20 | 26.7 | .219 |
| Diabetes mellitus | 15 | 20 | .536 |
| COPD | 11 | 14.7 | .047 |
| Kidney failure | 1 | 1.3 | .707 |
| Symptoms | |||
|---|---|---|---|
| Headache | 43 | 57.3 | <.0001 |
| Joint pain | 42 | 56 | .184 |
| Visual symptoms | 40 | 53.3 | .156 |
| General malaise | 40 | 53.3 | .059 |
| Temporal pain | 31 | 41.3 | <.0001 |
| Jaw claudication | 21 | 28 | .018 |
| Fever | 18 | 24 | .508 |
| Transient ischaemic attack | 10 | 13.3 | .371 |
| Death | 2 | 2.6 | .845 |
| Laboratory tests | |||
|---|---|---|---|
| Elevated ESR | 67 | 89.3 | .160 |
| Elevated CRP | 66 | 88 | .254 |
| Anaemia | 42 | 56 | .393 |
| Temporal Doppler ultrasound | 60 | 80 | |
| Temporal biopsy | 62 | 82.7 | |
| Positive biopsy | 31 | 50 | |
| ACR-SCORE ≥ 3 | 53 | 70.7 | <.0001 |
ACR-SCORE: American College of Rheumatology criteria; COPD: chronic obstructive pulmonary disease; CPR: C reactive protein; ESR: erythrocyte sedimentation rate; HT: hypertension.
P-value: calculated with the χ2 or Fisher’s exact test, considering a P-value <.05 statistically significant.
Symptoms were headache 43 cases (57.3%), joint pain 42 cases (56%), poor general condition 40 cases (53.3%), visual symptoms 40 cases (53.3%), temporal pain 31 cases (41.3%), jaw claudication 21 cases (28%), fever 18 cases (24%), transient ischaemic attack 10 cases (13.3%). In this study the presence of headache (P < .0001), temporal pain (P < .0001), and jaw claudication (P < .018) are statistically significant for diagnosis of TA.
DiagnosisFrom the laboratory findings, there was elevated ESR in 67 cases (89.3%) (P = .160) and elevated CRP in 66 cases (88%) (P = .254), with no statistical significance for diagnosis of TA. In the patients diagnosed with an ACR-SCORE ≥ 3, there was elevated ESR (65.04 ± 31.20 mm/h) and CRP (59.05 ± 45, 54 mg/l) compared to those without a diagnosis of TA, ESR (54 ± 34.3 mm/h) (P = .168) and CRP (50.29 ± 50.65 mg/l) (P = .465) (Table 2).
Behaviour of ESR and CRP values in the study.
| ACR-SCORE ≥ 3 | ACR-SCORE < 3 | P-value | Halo sign | No halo sign | P-value | Biopsy+ | Biopsy– | P-value | |
|---|---|---|---|---|---|---|---|---|---|
| ESR mm/h | 65.04 ± 31.20 | 54 ± 34.3 | .168 | 71.28 ± 27.50 | 45.59 ± 34.32 | .0066 | 70.58 ± 27.84 | 47.43 ± 34.69 | .015 |
| CRP Mg/l | 59.05 ± 45.54 | 50.29 ± 50.65 | .464 | 69.96 ± 44.26 | 37.81 ± 41.84 | .0255 | 70 ± 43.75 | 35.47 ± 40.17 | .007 |
ACR-SCORE: American College of Rheumatology criteria; CRP: C reactive protein; ESR erythrocyte sedimentation rate.
Temporal Doppler ultrasound was performed in 60 patients (80%), and the characteristic halo sign was observed in 32 cases (53.33%). Patients with a halo sign showed significantly elevated ESR and CRP compared to those without (halo ESR 71.28 ± 27.50 mm/h and no halo ESR 45.59 ± 34.32 mm/h [P = .0066] halo CRP 69;96 ± 44.26 mg/l and no halo CRP 37.81 ± 41.84 mg/l [P = .0255]).
Sixty-two (82.7%) patients underwent temporal biopsy, which was positive in 31 cases (50%). Of the 62 patients biopsied, 4% were insufficient samples (n = 3). The patients with positive biopsy had significantly higher CRP and ESR; (biopsy positive ESR 70.58 ± 27.84 mm/l versus 47.43 ± 34.69 mm/l (P = .015) and biopsy positive CRP 70 ± 43.75 mg/l versus 35.47 ± 40.17 mg/l [P = .007]).
TreatmentNinety-two percent (69 cases) of the patients were on corticosteroid treatment. Fifty-three patients (70.67%) had a positive diagnosis of TA, but 22 cases (29.33%), despite a negative diagnosis, remained on corticosteroids. Corticosteroids were discontinued in only 6 cases (8%).
All of the patients with a diagnosis of polymyalgia rheumatica (21) were on corticosteroids, and only 14 had a diagnosis of TA.
In this sample there were 2 deaths (P = .505), without statistical significance for the diagnosis of TA. The 2 cases (2.6%) were on corticosteroids (P = .845), and only one had a diagnosis of TA.
Economic studyFor the secondary objective, 47 patients with a median age of 76 years (46–87), 24 (51%) women, were included, who were the patients who underwent both temporal artery Doppler ultrasound and biopsy.
Total costs generated in this sampleIn this sample (n = 75), 60 temporal Doppler ultrasound scans were performed (10035.6) and 62 temporal biopsies (21064.5). The analysis of the cost generated by the diagnosis of TA in our centre is 414.7 per patient.
Costs generated using temporal biopsy: Table 3The cost of temporal artery biopsy is 339.75/patient. In this sample, temporal artery biopsy has a sensitivity of 33.33% (95% CI: 18.56%–50.97%) and a specificity of 0% (95% CI: .00%–28.49%) for diagnosis of TA, Table 3.
Relationship between anatomical pathology result and diagnosis (n = 47).
| Negative biopsy (absence of giant cells) | Positive biopsy (presence of giant cells) | Total | |
|---|---|---|---|
| ACR-SCORE < 3 | 11 (23.40%) | 0 (0%) | 11 (23.40%) |
| ACR-SCORE ≥ 3 | 12 (25.53%) | 24 (51.06%) | 36 (76.60%) |
| Total | 23 (48.93%) | 24 (51.06%) | 47 (100%) |
ACR-SCORE: American College of Rheumatology criteria.
Using the American College of Rheumatology criteria to diagnose TA with biopsy results in a saving of 18% compared to the diagnostic strategy we use in our hospital.
Costs generated using temporal Doppler ultrasound: Table 4The cost of Doppler ultrasound is 167.26 euros/patient. In our sample, this examination had a sensitivity of 58.33% (95% CI 40.76%–74.49%) and a specificity of 63.64% (95% CI 30.79%–89.07%) to diagnose TA, Table 4.
Relationship between temporal artery Doppler ultrasound result and diagnosis (n = 47).
| Negative Doppler ultrasound (absence of halo sign) | Positive Doppler ultrasound (presence of halo sign) | Total | |
|---|---|---|---|
| ACR-SCORE < 3 | 7 (14.98%) | 4 (8.51%) | 11 (23.40%) |
| ACR-SCORE ≥ 3 | 15 (31.91%) | 21 (44.68%) | 36 (76.60%) |
| Total | 22 (46.80%) | 25 (53.19%) | 47 (100%) |
ACR-SCORE: American College of Rheumatology criteria.
Using the ACR-SCORE to diagnose temporal arteritis with Doppler ultrasound imaging results in a saving of 59% compared to the diagnostic strategy we use in our hospital.
Costs generated when treatment was modified (discontinuation of corticosteroid): Table 5When assessing the cost of the corticosteroid discontinuation strategy, we would only have to perform biopsies or Doppler ultrasound when treatment has been discontinued. In the sample analysed (n = 47) treatment was only discontinued in 3 patients (6%); therefore, we would only have had to perform 3 biopsies, which represents a cost of 21.68/patient, or 3 Doppler ultrasounds, which represents a cost of 10.67/patient, and the saving varies from 94% to 97%, respectively, Table 5.
Relationship between treatment and diagnosis (n = 47).
| No treatment with corticosteroids | Treatment with corticosteroids | Total | |
|---|---|---|---|
| ACR-SCORE < 3 | 2 (4.16%) | 9 (19.15%) | 11 (23.40%) |
| ACR-SCORE ≥ 3 | 1 (2.13% | 35 (74.47%) | 36 (76.60%) |
| Total | 3 (6.38%) | 44 (93.62%) | 47 (100%) |
ACR-SCORE: American College of Rheumatology criteria.
Table 6 shows a comparison of the costs and savings using the different diagnostic strategies and change of treatment.
Comparison of the costs by the different strategies analysed and their savings.
| Total | AC and DU | AC and biopsy | Modify treatment and biopsy | Modify treatment and DU | |
|---|---|---|---|---|---|
| Sensitivity | 58.3% | 33.33% | 97.22% with 95% CI: 85.47%–99.93% | 97.22% with 95% CI: 85.47%–99.93% | |
| 95% CI: 40.76%–74.49% | 95% CI: 18.56%–50.97% | ||||
| Specificity | 63.6% | 0% | 18.18% with 95% CI: 2.28%–51.78% | 18.18% con 95% CI: 2.28%–51.78% | |
| 95% CI: 30.79%–89.07% | 95% CI: .00%–28.49% | ||||
| Euros/patient | 414.7 | 167.26 | 339.75 | 21.68 | 10.67 |
| Savings | 0% | 59.66% | 18.07% | 94.77% | 97.42% |
AC: American College of Rheumatology criteria; 95% CI: 95% confidence interval; DU: Doppler ultrasound.
TA is a disease that is of concern to physicians and patients in terms of diagnosis and potential relapses.11 Thorough history taking and clinical examination are still of paramount importance in its diagnosis.12 The symptoms and signs with the highest predictive value are visual symptoms (loss of vision or diplopia), new-onset headache, preauricular pain, jaw claudication, ESR greater than 50, and age over 50 years.2,11,13,14 In our series, headache, temporal pain, and jaw claudication were predictors of giant cell arteritis.
Smith et al.15 in 1997 were the first to use colour Doppler ultrasound to establish a diagnosis of TA. They concluded that there are some characteristic signs detectable with Doppler ultrasound, the most specific being the presence of a dark halo sign, secondary to oedema of the arterial wall. Since then, several studies have evaluated this technique, obtaining a sensitivity and specificity for the halo sign of 68%–69% and 81%–91% in the diagnosis of TA.16–18 In our study, the presence of halo sign has a sensitivity and specificity of 58.3% and 63.6%, respectively, for diagnosis of TA, which differs from the published results; this is because the presence of a halo sign is compared with positive pathological anatomy and not with diagnosis according to an ACR-SCORE greater than 3. However, for González Porto et al.19 who compare ultrasound with clinical findings, sensitivity is 42.6% and specificity is 65.7%, which are results more similar to those obtained in our study. However, this was not the aim of our study.
Some authors suggest that in the case of a high pretest probability (clinical and analytical), a pathological Doppler may be sufficient to diagnose TA, without the need for a biopsy.11,12,20,21 In this study, elevated ESR and CRP are predictors of a positive biopsy or presence of a halo sign on ultrasound, and therefore diagnosis of TA.
The sensitivity of temporal artery biopsy can be as low as 39%, and about 7% of all temporal artery biopsies may not actually consist of arterial tissue.22 In our work the biopsy yielded a sensitivity of 33% and only 4% of the samples were insufficient. The positivity of temporal artery biopsy depends on the size, with biopsies smaller than .5 cm the yield is low and those larger than 2 cm in length tend to be high yield.2 It was not the aim of this study to determine the length of the temporal artery analysed. In the study by González-Gay et al.,23 190 patients were diagnosed with TA; the best predictive model for biopsy-proven TA included a history of constitutional syndrome (OR = 6.1), an abnormal temporal artery on physical examination (OR = 3.2), and the presence of visual complications (OR = 4.9). A subset of patients had a high probability of a negative temporal artery biopsy, but met the 1990 ACR classification criteria for TA when they were applied. This subset with negative temporal artery biopsy had less severe ischaemic complications than those with biopsy-proven GCA. Thus, in patients without visual manifestations, with a normal temporal artery on physical examination and without constitutional syndrome, the risk of having an abnormal temporal artery biopsy was low.23
Many temporal artery biopsies are negative, less than 60% of patients with clinical temporal arteritis have a positive biopsy,11,13,24,25 in our work only 50% of biopsies were positive, we consider it essential like Gajree et al.13 and Lyons et al.,11 to find ways to reduce the number of patients undergoing unnecessary biopsy, to reduce workload and optimise services. It is no longer standard clinical practice, due to the use of temporal artery ultrasound, to perform a second contralateral biopsy in patients with a high suspicion of GCA, as it increases the biopsy yield by 10%.26 This study demonstrates that there are clinical factors (headache, temporal pain, and jaw claudication) and analytical factors (elevated ESR and CRP) already described by other authors, such as González-López12 who present a tool such as the calculator (logistic regression analysis) that can help predict the outcome of the biopsy, help improve clinical decision-making, and avoid unnecessary biopsies.10
The cost-effectiveness study by Luqmani et al.21 indicates that ultrasound alone is more cost-effective than biopsy alone, largely due to its much lower cost (58 versus £514) and higher sensitivity (54% versus 39%), in our work there is also an ostensible difference between the 167.26 for Doppler ultrasound and 339.75 for biopsy and we have similar results for sensitivity (58% versus 33%). If we compare this with the cost incurred in our hospital (414/patient) (many patients undergo both biopsy and Doppler ultrasound), we are talking about a saving ranging from 59% to 18%.
If we follow the most cost-effective strategy, we would rely on ultrasound and clinical judgement alone as a means of diagnosis.21 The rationale behind the additional use of biopsy, despite a negative scan, would be to provide further evidence to rule out disease, and to support discontinuation of therapy in the event that both tests are negative.2,20,21 Brabyn et al.14 report corticosteroid maintenance in 70%–75% of patients, which is comparable to our study, where only 6% of our patients were withdrawn from corticosteroid therapy. In this study, 29.3% of patients were kept on corticosteroids despite a negative diagnosis. A reason for this could be that 28% of the patients had a diagnosis of polymyalgia rheumatica. Also, in our study there were 2 deaths, and both were taking corticosteroids at high doses, although mortality and potential complications were not the aim of this study.
It has already been published that the use of a pre-test clinical probability pathway and non-crucial diagnostic tests to initiate early treatment and prevent vision loss are cost-effective strategies,11,12,21 which we fully agree with. We must be aware of the costs generated by our actions and even potential complications for patients. With this study, we can conclude that when clinical and laboratory data are available, a diagnosis of TA can be made, leaving biopsy for those patients in whom we wish to discontinue corticosteroids, i.e., not performing a biopsy when we know that we are not going to discontinue corticosteroids.
Work is needed to validate the predictive calculator.
LimitationsThis is a retrospective study, the quality of life of the patients was not assessed, and neither were the length of the biopsied artery, complications from the biopsy, potential complications of long-term treatment with corticosteroids, or mortality considered.
ConclusionsIn our population, the presence of headache, temporal pain, and jaw claudication are predictors of giant cell arteritis. Elevated ESR and CRP are predictors of positive biopsy and presence of halo sign on ultrasound.
ACR-SCORE ≥ 3 with Doppler ultrasound or biopsy, as well as diagnosis with discontinuation of corticosteroids are cost-effective.
FundingThe present research received no specific support from public sector agencies, commercial sector, or non-profit entities.
Conflict of interestsThe authors have no conflict of interests to declare.