To investigate, in Spanish patients with rheumatic diseases treated with subcutaneous biological drugs, their sources of information, which sources they consider most relevant, and their satisfaction with the information received in the hospital.
MethodsRheumatologists from 50 hospitals handed out an anonymous survey to 20 consecutive patients with rheumatoid arthritis, axial spondyloarthritis or psoriatic arthritis treated with subcutaneous biologicals. The survey was developed ad hoc by 4 rheumatologists and 3 patients, and included questions with closed-ended responses on sources of information and satisfaction.
ResultsThe survey was handed-out to 1000 patients, 592 of whom completed it (response rate: 59.2%). The rheumatologist was mentioned as the most important source of information (75%), followed by the primary care physician, nurses, and electronic resources; 45.2% received oral and written information about the biological, 46.1% oral only, and 6.0% written only; 8.7% stated that they had not been taught to inject the biological. The percentage of patients satisfied with the information received was high (87.2%), although the satisfaction was lower in relation to safety. If the information came from the rheumatologist, the satisfaction was higher (89.6%) than when coming from other sources (59.6%; P<.001). Satisfaction was also higher if the information was provided orally and written (92.8%) than if provided only orally (86.1%; P=.013); 45.2% reported having sought information from sources outside the hospital.
ConclusionsThe rheumatologist is key in transmitting satisfactory information on biological treatment to patients. He or she must also act as a guide, since a high percentage of patients seeks information in other different sources.
Conocer las fuentes de las que los pacientes españoles con enfermedades reumáticas tratados con fármacos biológicos subcutáneos obtienen información, cuáles consideran más relevantes y su satisfacción con la información recibida en el hospital.
MétodosReumatólogos de 50 hospitales entregaron una encuesta anónima, desarrollada ad hoc por 4 reumatólogos y 3 pacientes, a 20 pacientes consecutivos con artritis reumatoide, espondiloartritis axial o artritis psoriásica tratados con biológicos subcutáneos. La encuesta incluyó preguntas con respuestas cerradas sobre los aspectos mencionados previamente.
ResultadosRecibieron la encuesta 1.000 pacientes, 592 la devolvieron cumplimentada (tasa de respuesta: 59,2%). El reumatólogo fue mencionado como la fuente de información más importante (75%), seguido del médico de atención primaria, la enfermería y los recursos electrónicos. El 45,2% recibió información oral y por escrito sobre el biológico, el 46,1% solo oral, el 6% solo por escrito. Un 8,7% declaró no haber sido enseñado a inyectarse el biológico. El porcentaje de pacientes satisfechos con la información recibida fue elevado (87,2%), aunque la satisfacción fue menor en temas relacionados con la seguridad. Si la información provenía del reumatólogo, la satisfacción era mayor (89,6%) que cuando provenía de otras vías (59,6%; p<0,001). La satisfacción también era mayor si se dio oral y por escrito (92,8%) frente a solo oral (86,1%; p=0,013). Un 45,2% declaró haber buscado información en fuentes fuera del hospital.
ConclusionesEl reumatólogo es clave a la hora de transmitir información satisfactoria al paciente en tratamiento biológico. Debe además actuar de guía, ya que un elevado porcentaje busca información en fuentes distintas.
There is no doubt that the biological agents have revolutionised the treatment of inflammatory rheumatic diseases. Either directly or through better knowledge of the disease as a result of the enormous amount of research that has led to their use in rheumatology, unprecedented objectives have been met in the control of the disease. Never before have so many effective therapeutic alternatives been available to us. However this fact, positive in principle, could lead to situations of uncertainty or indecision for certain patients.1
Because there are alternatives, it is essential for patients to be able to voice their opinion and preferences in order to facilitate decisions and ensure their adherence to prescribed treatment.2–8 However, to do so they require judgement, which means they must be appropriately informed about their disease and its treatment.9–11
The barometer of the platform EsCrónicos, completed in 2014, on access to quality care of Spanish patients with chronic disease, showed that 60% of respondents considered the information provided them on their disease and other aspects of daily life a priority for improvement in the National Health System.12 In the field of rheumatology, several papers have covered the desire of patients for more information on their disease, and for practitioners to consider their preferences when deciding treatment.13,14 Nonetheless, these research studies in the area of rheumatology have only been undertaken in English-speaking countries and might not reflect the situation in our country. Furthermore, they do not provide details about the information on the biological drugs, frequently acquired from the media and social networks. Patients can, therefore, receive information from unexpected sources, and this can have undesirable effects.15
This is why we set out to study how Spanish patients with inflammatory disease under treatment with biologicals perceive the information they receive about their biological treatment, their information sources, and their satisfaction with the information they have received in hospital.
MethodsRHEU-LIFE was a survey conducted between September and October 2015 on patients with inflammatory rheumatic diseases treated with subcutaneous (sc)biologicals. We limited the survey to sc biologicals because there is evidence that there is a greater adherence problem with these than those administered intravenously,16–18 and there are problems with administration associated with the information received (because the information on the method of administration of intravenous drugs is received by the nurse who administers the drug). The patients were invited to participate by rheumatologists from 50 Spanish hospitals. Adult patients diagnosed with one of 3 target diseases were selected: rheumatoid arthritis, axial spondyloarthritis and psoriatic arthritis. The patients had to have been treated with sc biologics at least since their last medical consultation and, in the opinion of the rheumatologist, had to be able to understand and respond to the survey. The survey was delivered by hand, printed, to the first 20 consecutive patients with the abovementioned features who attended outpatient clinics routinely, regardless of their age, sex, disease duration or severity in the days that the survey was open.
The patients were given a sealed envelope containing the printed survey and printed information about the purpose of the survey. They were informed that their participation was voluntary, and that they were free to answer all or some of the questions. The content of the survey ensured that it was impossible to identify the respondents, thus guaranteeing anonymity. The patients were asked to respond, if they decided to do so, from their homes and to return the questionnaire in a pre-aid envelope directly to the agency in charge of the compilation and analysis of the data. The patients were not sent reminders and no clinical data was gathered from clinical records.
Survey FormThe survey content was developed ad hoc for the RHEU-LIFE project with the participation of 4 rheumatologists experienced in the care of patients with rheumatic diseases and in research methodology, and was reviewed and completed with the suggestions of 3 patients from the patient's association Conartritis (National Arthritis Coordinator), to ensure the suitability of the questions and the language used. The final survey comprise 54 questions with closed-ended response options that included the following: basic demographic features, perception of the impact of the disease on daily life, aspects relating to how patients receive information about the disease and the treatments, what they expect from the medication, and their satisfaction with their current treatment, plus some aspects on the logistics of dispensing the sc biological drug and follow-up in hospital. The results on the perception of impact and satisfaction with treatment have been described previously.19
This article focuses on aspects relating to patient information. To establish their sources of general information about the disease, the patients highlighted options from a closed list that included hospital staff, other healthcare centres, social networks and the media. They could mark all the options they wanted, and also highlight which they considered most important. With regard to the information they received on treatments in general, and on biological treatment in the hospital in particular, the patient could highlight various options from “the rheumatology specialist”, “nursing staff”, “the hospital pharmacy”, “other source”, “I don’t remember” or “nobody has given me information”.
Their level of satisfaction with the information received in the hospital on the sc biological drug was rated by the patient as “very satisfied”, “quite satisfied”, “neither satisfied nor dissatisfied”, “dissatisfied” or “very dissatisfied”. Finally, taking all their sources into account, the patients assessed themselves as having been “well informed”, “adequately informed”, “poorly informed” or “not informed at all”, and they answered various questions from the Satisfaction with Information about Medicines Scale.20
Statistical AnalysisThis survey is considered exploratory in nature and therefore no hypothesis was formulated nor was there a formal calculation of the sample size. No imputation was made on missing values either. The variables are expressed in means and standard deviation, and the qualitative variables in percentages. The comparisons between percentages with respect to different variables (age ranges, sex, baseline disease and others) were made with the chi-squared or Fisher's exact test. With regard to these comparisons, the categories “very satisfied” and “quite satisfied” were grouped into one category, whereas the perceived degree of information was grouped as “well/adequately informed “and “poorly/not informed at all”. A P value .05 or less was considered statistically significant. The statistical software SPSS, version 18.0.0, was used for the data processing.
Ethical ConsiderationsThe survey and the working procedures were reviewed and approved by the Ethics Committee of Madrid's Gregorio Marañón University Hospital, and the ConArtritis patients’ association.
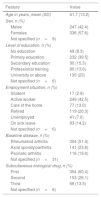
ResultsBetween September and October 2015, 1000 patients were given the survey, and 592 returned it completed (response rate: 59.2%). The demographic features of the respondents are summarised in Table 1. The sc biological drug with which the patients were treated was the first for 60.4%, the second for 26.1%, and the third or more for 13.5%.
Features of the Patients Who Responded to the RHEU-LIFE Survey.
| Feature | Value |
|---|---|
| Age in years, mean (SD) | 41.7 (13.2) |
| Sex, n (%) | |
| Males | 247 (42.4) |
| Females | 336 (57.6) |
| Not specified (n=9) | |
| Level of education, n (%) | |
| No education | 49 (8.3) |
| Primary education | 232 (39.5) |
| Secondary education | 90 (15.3) |
| Professional training | 80 (13.6) |
| University or above | 135 (23) |
| Not specified (n=6) | |
| Employment situation, n (%) | |
| Student | 17 (2.9) |
| Active worker | 249 (42.5) |
| Care of the home | 77 (13.0) |
| Retired | 119 (20.3) |
| Unemployed | 41 (7.0) |
| On sick leave | 83 (14.2) |
| Not specified (n=6) | |
| Baseline disease, n (%) | |
| Rheumatoid arthritis | 304 (51.4) |
| Axial spondyloarthritis | 141 (23.8) |
| Psoriatic arthritis | 116 (19.6) |
| Not specified (n=31) | |
| Subcutaneous biological drug, n (%) | |
| First | 354 (60.4) |
| Second | 153 (26.1) |
| Third | 69 (13.5) |
| Not specified (n=6) | |
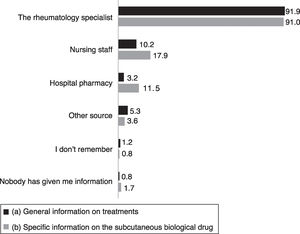
Table 2 shows the principal information sources on rheumatic disease mentioned by the patients. In addition to the rheumatology specialist, considered the most important source, the patients mentioned their primary care physician and nursing staff, and frequently electronic resources (Table 2). With regard to the information received on the treatments in general, and on biological treatment in particular, more than 90% responded that they received information from the rheumatology specialist, and much less frequently from nursing staff and the hospital pharmacy (Fig. 1). Forty-five point two percent had received information about the biological drug orally and in writing, 46.1% only orally, 6% only in writing. Eighty-four point five percent mentioned having been trained how to inject the drug, a family or friend of 6.8% had been trained, and 51 patients (8.7%) claimed that they had received no training at all.
Sources of Information on Rheumatic Disease.
| (a) Sources of information | (b) Most important source | |
|---|---|---|
| Primary care physician | 128 (21.6) | 24 (4.1) |
| Specialist (rheumatologist) | 442 (74.7) | 442 (74.8) |
| Nursing staff | 114 (19.3) | 4 (.7) |
| Pharmacist | 20 (3.4) | 1 (.2) |
| Websites specialising in rheumatic diseases | 117 (19.8) | 6 (1) |
| Disease or health blogs | 33 (5.6) | 1 (.2) |
| Friends of family members | 37 (6.3) | 1 (.2) |
| Mainstream media (press, television or radio) | 29 (4.9) | 0 (0) |
| Patient brochures | 68 (11.5) | 1 (.2) |
| Patients’ association | 26 (4.4) | 0 (0) |
| Other patients | 18 (3) | 0 (0) |
| Other | 1 (.2) | 0 (0) |
| Did not respond | 2 (.3) | 112 (18.9) |
The information is presented as n (%). (a) Patients’ main sources of information on their disease (the patients were able to mark all the options they wanted), (b) Source mentioned by the patient as their most important source (the patients were only able to mark one).
When the patients were asked about their satisfaction with the information received in hospital on the sc biological treatment that they were using, 87.2% claimed that they were satisfied (44.5% very satisfied and 42.6% quite satisfied), 10.6% were neither satisfied nor dissatisfied, and 2.3% were dissatisfied. The level of satisfaction did not depend on whether the patient was on their first, second or third biological, or their diagnosis (P>.05). The percentage of those who were satisfied/very satisfied was less when it not been the rheumatologist who had informed the patient (59.6 vs 89.6% when it had: P<.001). For the patients who had received verbal and written information, the percentage of satisfied/very satisfied was higher (92.5%) than when only oral information had been received (86.1%; P=.013).
Search for Information From Sources Other Than Hospital StaffForty-five percent of the patients mentioned having sought information on the biological drug from sources other than the hospital's healthcare staff. Table 3 shows the percentages according to the demographic features. It was most often the younger patients, with higher levels of education, or those treated with a first biological drug that had turned to information sources other than healthcare staff. No association was seen between looking to other sources and the format in which they had received the information in hospital (42.5% verbal, 49.2% in writing; P=.121), or with their satisfaction with the information received in hospital (45.5%of those who were quite/very satisfied with the information, and 44% of those who were dissatisfied had sought information from other sources; P=.455).
Percentage of Patients Who Responded “Yes” to the Question “Have You Looked for Information on Subcutaneous Biological Treatment From Sources Other Than Hospital Staff (e.g., Websites, Patients’ Associations or Others)?
| Patient features | Looked for information outside the hospital (%) | P |
|---|---|---|
| Age (quartiles) | ||
| <43 years (n=141) | 92 (65.2) | <.001 |
| 43–52 years (n=144) | 74 (51.4) | |
| 53–62 years (n=133) | 52 (39.1) | |
| ≥62 years (n=131) | 27 (20.6) | |
| Sex | ||
| Males (n=245) | 115 (46.9) | .499 |
| Females (n=332) | 146 (44) | |
| Level of education | ||
| No education (n=49) | 7 (14.3) | <.001 |
| Primary education (n=228) | 72 (31.6) | |
| Secondary education (n=90) | 50 (55.6) | |
| Vocational training (n=79) | 47 (59.5) | |
| University or above (n=134) | 87 (64.9) | |
| Baseline disease | ||
| Rheumatoid arthritis (n=301) | 133 (51.6) | .173 |
| Axial spondyloarthritis (n=141) | 75 (53.2) | |
| Psoriatic arthritis (n=114) | 50 (43.9) | |
| Subcutaneous biological drug | ||
| First (n=351) | 175 (49.9) | .014 |
| Second (n=151) | 57 (37.7) | |
| Third (n=78) | 49 (37.2) | |
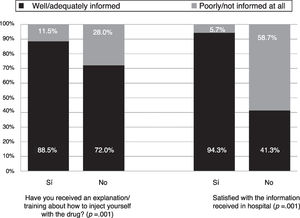
Forty-two percent of the patients declared that, with all the information that they had, they felt well informed about the characteristics of the sc biological drug, 44.7% felt they were adequately informed, 12.1% poorly informed and .7% not informed at all. The percentages of patients who considered themselves well or adequately informed were similar in terms of age ranges, sex, educational level, baseline disease and order of biological drug. The percentage considering themselves well/adequately informed was even higher when the information on the biological had been received in both forms, verbally and in writing (92.8%) compared to when it had only been received orally (80.0%; P=.037). More patients perceived themselves as poorly or not informed were not satisfied with the information received in hospital, and those who had not been trained on how to inject the drug (Fig. 2).
Perception of the level of general information reported by the patients. Responses to the question “Considering all the information that you have, how would you rate the information you have received about the subcutaneous biological drug you are currently injecting?” The percentage of patients that responded “well/adequately informed” compared to “poorly/not at all informed” according to their satisfaction with the information received in hospital and whether they had been informed/trained on how to administer the biological drug.
Finally, the patients were asked about the level of information regarding certain aspects of their biological treatment (Table 4). The majority responded that they had received an adequate level of information. However, around a third mentioned that they had been given little or no information on essential aspects such as the type of adverse events associated with the drug, the risk of experiencing them and what to do if they did.
Patients’ Responses to the Question “What do You Think About the Information You Have Received on…?”.
| Too much information | Adequate information | Poor information | I have not received information | I don’t need it | |
|---|---|---|---|---|---|
| What your treatment does (n=559) | 23 (4.1) | 448 (80.1) | 68 (12.2) | 16 (2.9) | 4 (.7) |
| How long it takes to act (n=527) | 16 (3) | 353 (67) | 112 (21.3) | 43 (8.2) | 3 (.6) |
| How you can know if it is working (n=527) | 19 (3.6) | 349 (66.2) | 110 (20.9) | 40 (7.6) | 9 (1.7) |
| How much time it will take for your medicine to take effect (n=516) | 17 (3.3) | 329 (63.8) | 115 (22.3) | 49 (9.5) | 6 (1.2) |
| How to use your medicine (n=525) | 47 (9.0) | 440 (83.8) | 27 (5.1) | 6 (1.1) | 5 (1) |
| Adverse effects associated with the drug (n=527) | 29 (5.5) | 326 (61.9) | 124 (23.5) | 43 (8.2) | 5 (.9) |
| Risk of suffering adverse effects (n=529) | 33 (6.2) | 304 (57.5) | 140 (26.5) | 49 (9.3) | 3 (.6) |
| What to do if you experience an adverse effect (n=527) | 22 (4.2) | 314 (59.6) | 126 (23.9) | 61 (11.6) | 4 (.8) |
| What to do if you forget to take a dose of your medication (n=525) | 31 (5.9) | 377 (71.8) | 71 (13.5) | 37 (7) | 9 (1.7) |
The number and percentage of responses to each question is shown in brackets.
The RHEU-LIFE study explored the perception and satisfaction of rheumatic patients treated with sc biological drugs in terms of the information received, necessary to include patients in decision-making. The results show that the rheumatologist is crucial in ensuring that patients receive appropriate information on their disease and its treatments, even though they can use additional information sources, in which case the rheumatologist is even more important as a guide to safe information sources.
The rheumatologist plays such an important role in patients’ satisfaction with the information received that satisfaction clearly reduces when they are not the source of their information. Confidence in the physician is defined as “the belief or trust that the physician will provide reliable information and act in the interest of the patient”.21 Trust is very important to achieve appropriate adherence and good treatment outcome, and is enhanced by effective communication.22,23 Self-efficacy and healthcare literacy are also crucial to adherence, and both require information and education.24,25 A meta-analysis confirmed that communication in health is highly correlated with better patient adherence, and that training in communication and information techniques for doctors improves adherence.26 However, physicians in general and rheumatologists in particular, have limited training in communication and information skills, although better than other specialities.27
Although the RHEU-LIFE survey highlighted that the more information formats (oral and written) the greater the satisfaction, additional information in writing only slightly increases satisfaction in absolute terms, yet it does so significantly. In general it is known that visual aids – written information or educational pamphlets – do not appeal to patients with a low level of health literacy, since they contain a lot of numbers and few pictures.28 In general we recommend that information should be adapted to the patient; this is easier to achieve in principle if it is the doctor who decides what to explain and how to explain it.
Nevertheless, the messages used by rheumatologists might be biased and repeated until they become the norm, as argued in an article by Pincus et al., which states that information that is routinely given on a drug commonly used in rheumatology, methotrexate,29 is largely erroneous,30 and needs to be revised.
Regardless of their satisfaction with the information and how it was given, a significant number of patients sought information about the biological drug from sources other than health professionals. Although this is not altogether negative, it is important to guide patients towards safe sources of information, e.g., patient websites of scientific societies or patients’ associations – which will reduce the risk of losing therapeutic adherence or erroneous beliefs or thoughts about the disease or its treatment, as has occurred with other treatments,15 resulting in extreme cases such as failing to adhere to vaccination schedules.31
Although the difference was not significant, more of the patients considered that information on adverse effects and how to manage them was insufficient. It is not clear whether doctors really provided the information or whether they avoided doing so thus negatively affecting adherence. It is obvious that patients require this information13 and it is crucial for shared decision-making. In the ARCO study, more than 70% of patients with rheumatoid arthritis under sc biological treatment felt concerned about the long-term effects of the medication.32 Moreover, not knowing what might occur a priori might result in a failure to report safety problems.33
This study has its limitations. Because it was an anonymous study, the profile of the patients who did not respond was not known, and we cannot form a judgement on how the patients really received their information. The response rate (59.2%) is similar to that described in other surveys using a similar methodology.34,35 An additional limitation might be the fact that all the patients were taking biological medication. It was seen that the expectations of improvement when taking a biological is very high,36,37 and it is possible that the fact that the patients were taking these treatments predisposed them to evaluate the information received from the doctor as satisfactory. This might also mean that other sources of information did not seem to be relevant for the patients. In particular, the small amount of information they received from nurses or the pharmacy is striking. Curiously, both healthcare groups had been better trained in health education and how to give information on medication than the doctors themselves, many of whom had no access even to injection devices to be able to explain how to use them to patients. It is possible that they have no time to do so during the medical consultation. Although the amount is very low, it is striking that one patient had not received information on the biological, and that they had not been taught how to self administer it. It is not possible for us to check this, but perhaps this is happening in hospitals where there are no rheumatology nurses or where there are no patient education protocols. This lack of information and training might result in lower adherence, lower blood levels of the drug or even adverse effects.38 On the other hand, we did not specifically validate the concrete questions on the information received, although they were based on items that are widely used in surveys of this type.
In conclusion, the RHEU-LIFE survey has highlighted the importance of the rheumatologist and their communication skills in informing and guiding patients in their healthcare education, and discussing with them expectations in terms of efficacy, tolerability and short and long-term side effects.
Conflict of InterestsLuis Cea-Calvo, María J. Arteaga and Sabela Fernández are full time employees of Merck Sharp & Dohme, Spain. The rest of the authors received honoraria as consultants in the design, implementation and interpretation of the study data. Enrique Battle-Gualda has been a consultant for Roche, BMS and MSD and has received honoraria as speakers from Abbvie, UCB, Roche, Pfizer, and BMS. Carlos M González has received honoraria as a speaker from MSD. The remaining authors have no conflict of interests to declare
This project was financed by Merck Sharp & Dohme, Spain, a subsidiary of Merck & Co., Inc., Kenilworth, New Jersey, U.S.A. and was reviewed and endorsed by the ConArtritis patients’ association (National Arthritis Coordinator). The data analysis was performed by Alejandro Pedromingo (www.bio-estadistica.com).
We would like to acknowledge the work of the healthcare professionals who helped in delivering the survey to the patients, and particularly the patients for their collaboration in completing and returning the surveys.
The healthcare professionals who facilitated the RHEU-LIFE survey were as follows (in alphabetical order): Pilar Ahijado Guzmán (Hospital Infanta Elena, Madrid), Javier Alegre López (Hospital Universitario de Burgos), Andrés Ariza Hernández (Hospital General de Ciudad Real), Emilia Aznar (Hospital Lozano Blesa, Zaragoza), Joaquín Belzunegui (Hospital Universitario de Donostia, San Sebastián), Daniel Batista Perdomo (Hospital Insular, Las Palmas de Gran Canaria), Juan Carlos Bermell Serrano (Hospital Virgen de la Luz, Cuenca), Pilar Bernabeu (Hospital San Juan, Alicante), María Bonet (Hospital l‘Alt Penedés, Vilafranca), Vanesa Calvo del Río (Hospital Marqués de Valdecilla, Santander), Benita Cardona Natta (Hospital Mateu Orfila, Menorca), Carmen Carrasco Cubero (Hospital Universitario Infanta Cristina, Badajoz), Natalia Casasnovas Pons (Centro de Salud Canal Salat, Menorca), Iván Castellvi (Hospital l‘Alt Penedés, Vilafranca), Rosa Castillo Montalvo (Hospital Universitario de Guadalajara), Virginia Coret Cagigal (Hospital Carlos Haya, Malaga), Ana Cruz Valenciano (Hospital Severo Ochoa, Madrid), Carlos Fernández López (Hospital Universitario A Coruña), Fernando Gamero Ruiz (Hospital Virgen del Puerto, Plasencia), Blanca García (Hospital San Jorge, Huesca), Rosa García Portales (Hospital Virgen de la Victoria, Málaga), Javier R. Godo (Especialista en Reumatología, Madrid), Antonio Gómez (Hospital Parc Taulí, Sabadell), Amparo Gómez Cañadas (Hospital Mutua de Terrassa), Silvia Iniesta Escolano (Hospital del Mar, Barcelona), Ana María Jiménez (Hospital Infanta Sofía, Madrid), Cristina Lerín Lozano (Hospital Manacor, Mallorca), Juan José Lerma (Hospital General de Castellón), María López Lasanta (Hospital Vall d́Hebrón, Barcelona), Pilar Morales Garrido (Hospital Virgen de las Nieves, Granada), Estefanía Moreno (Hospital l‘Alt Penedés, Vilafranca), María José Moreno (Hospital Rafael Méndez, Lorca), Jose Antonio Mosquera (Complejo Hospitalario de Pontevedra), Alejandro Muñoz Jiménez (Hospital Virgen del Rocío, Sevilla), Cristóbal Núñez-Cornejo (Hospital Universitario La Fe, Valencia), Alejandro Olivé (Hospital Germans Trias i Pujol, Barcelona), Carmen Ordás Calvo (Hospital de Cabueñes, Gijón), Rafaela Ortega Castro (Hospital Reina Sofía, Córdoba), Fred Antón Pagés (Hospital Río Carrión, Palencia), Eva Pérez Pampín (Complejo Hospitalario Universitario de Santiago de Compostela), Lucía Pantoja Zarza (Hospital del Bierzo, León), Manuel Riesco Díaz (Hospital Juan Ramón Jiménez, Huelva), Fernando Rodríguez (Hospital Santa Lucía, Cartagena), Sergio Rodríguez Montero (Hospital Nuestra Señora de Valme, Seville), Ana Rubial (Hospital de Txagorrituxu, Alava), Carmen Rusiñol (Hospital Mútua de Terrassa), Celia Saura Demur (Hospital Clinic, Barcelona), Beatriz Tejera Segura (Hospital Universitario La Laguna, Tenerife), Carlos Tomás (Hospital Mora d́Ebre, Tarragona), Carmelo Tornero (Hospital Morales Meseguer, Murcia), Pilar Trenor (Hospital Clínico de Valencia), Larissa Valour (Hospital Universitario Gregorio Marañón, Madrid), Amparo Ybáñez (Hospital Dr. Peset, Valencia).
Please cite this article as: de Toro J, Cea-Calvo L, Battle E, Carmona L, Arteaga MJ, Fernández S, et al. Percepciones de los pacientes con enfermedades reumáticas tratados con biológicos subcutáneos sobre su nivel de información. Encuesta RHEU-LIFE. Reumatol Clin. 2019;15:343–349.