To explore the patient journey of people with fibromyalgia (FM) in Latin American countries in order to identify problems in health care and other areas that may be resolvable.
MethodsQualitative study with phenomenological and content analysis approach through focus groups and patient journey (Ux; User Experience) methodology. Nine virtual focus groups were conducted with FM patients and healthcare professionals in Argentina, Mexico and Colombia recruited from key informants and social networks.
ResultsForty-three people participated (33 were clinicians and 10 were patients). The agents interacting with the patient in their disease journey are found in three spheres: healthcare (multiple medical specialists and other professionals), support and work life (including patient associations) and socioeconomic context. The line of the journey presents two large sections, two loops and a thin dashed line. The two major sections represent the time from first symptoms to medical visit (characterized by self-medication and denial) and the time from diagnosis to follow-up (characterized by high expectations and multiple contacts to make life changes that are not realized). The two loop phases include (1) succession of misdiagnoses and mistreatments and referrals to specialists and (2) new symptoms every so often, visits to specialists, diagnostic doubts, and impatience. Very few patients manage to reach the final phase of autonomy.
ConclusionThe journey of a person with FM in Latin America is full of obstacles and loops. The desired goal is for all the agents involved to understand that self- management by the patient with FM is an essential part of success, and this can only be achieved with early access to resources and guidance from professionals.
Explorar la experiencia de las personas con fibromialgia (FM) en países latinoamericanos con objeto de identificar problemas en la atención sanitaria y otros ámbitos potencialmente solucionables
MétodosEstudio cualitativo con enfoque fenomenológico y de análisis de contenido a través de grupos focales y metodología de viaje del paciente (Ux del inglés User Experience). Se llevaron a cabo 9 grupos focales virtuales con pacientes con FM y profesionales sanitarios en Argentina, México y Colombia reclutados a partir de informantes clave y redes sociales
ResultadosParticiparon 43 personas (33 clínicos y 10 pacientes). Los agentes que interaccionan con el paciente en la enfermedad se encuentran en tres esferas: la de la atención sanitaria, la del apoyo y vida laboral y la del contexto socioeconómico. La línea del viaje presenta dos grandes tramos, dos bucles y una línea discontinua delgada. Los dos grandes tramos representan los tiempos que van desde los primeros síntomas hasta la visita médica y desde el diagnóstico hasta el seguimiento. Los bucles incluyen 1º) sucesión de diagnósticos, tratamientos erróneos y derivaciones a especialistas y 2º) nuevos síntomas cada cierto tiempo, visitas a especialistas y dudas diagnósticas. Pocos pacientes logran la fase final de autonomía
ConclusiónEl viaje de una persona con FM en Latinoamérica está lleno de obstáculos. La meta deseada es que todos los agentes entiendan que el automanejo por parte del paciente con FM es una parte indispensable del éxito, y sólo se puede lograr accediendo a recursos de forma precoz y guiado por profesionales
Fibromyalgia (FM) is a chronic disease characterised by chronic pain, with a prevalence between .5% and 5.0%,1 which affects women between 2 and 7 times more than men.2 It is characterised by chronic generalised pain to which other non-specific symptoms are added, such as sleep disturbances, fatigue, joint stiffness, concentration problems, headaches or migraines, paresthesias and irritable bladder or bowel, among others.3
The presence of FM has a great impact on the quality of life of the individuals who suffer from it and on their development at a personal, family and social level, which leads to breakups, additional family obligations and even economic losses both for health and care costs as well as labour costs, often leading to employment disability.4 The economic impact of FM on employment is notable, to the point that almost half of patients missed at least 2 weeks of work in the last year due to FM, almost a quarter, in fact, were unable to work at all, and another quarter were unable to work full time because of FM.5,6
Although FM is the most common chronic widespread pain condition, it is often underdiagnosed,7 despite the fact that diagnosing FM has been shown to not only increase patient satisfaction8 but also reduce healthcare resource utilisation and care attendance.9 It could even be highlighted that FM is often incorrectly perceived as a "diagnosis of exclusion", which one is reluctant to reach.10
Much is known about FM, including its possible causes, the pain mechanisms involved, the long-term prognosis, and even which treatments are effective and which are not. However, the wide range of health professionals that people with FM see generally stand out for having limited or biased knowledge of the disease and options for its management.11–13
To date, research has largely focused on diagnosis and treatments; leaving aside organisational aspects of care for people with FM. This evidence gap was highlighted in the European Alliance of Rheumatology Associations (EULAR) recommendations on FM management updated in 2017.14
European and Latin American healthcare environments differ. A survey conducted in these 2 regions15 found that, in Europe, people with FM are more frequently treated in primary care than in specialised care, compared to only 32% of residents in Latin American countries. The ability to perform an efficient and accurate assessment and diagnosis depends on the doctor's prior knowledge and training, and differences in training between countries may have influenced patients' journey to diagnosis.16,17 Likewise, advances in understanding the pathophysiology of FM may not have extended to primary care specialists, and may also differ between regions, e.g., as indicated by differences in knowledge and adoption of criteria from the American College of Rheumatology (ACR).
When improving care for any disease, it is important to identify problems and needs, as well as where clinical practice deviates from evidence-based recommendations and why. This is why a qualitative evaluation is justified in this context analysis. The objective of this study is to explore the events in the journey or experiences of people with FM in Latin American countries, from the beginning of the symptoms to the diagnosis, and subsequent experience with the disease, the relationship between people with FM and the health professionals, the management of the disease (monitoring, treatments, referrals) and possible events with the health system, with the ultimate goal of identifying problems in health care and in the social and work sphere, and other areas that may be resolvable.
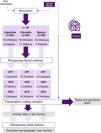
MethodsA qualitative study was carried out with a phenomenological approach and content analysis through focus groups. Fig. 1 shows the phases of the study and the participation rate in each one.
Study populationThere were 2 types of participants, one with an experiential perspective (people with FM aged over 18 years) and another with an expert perspective (health professionals who care for people with FM). For its selection, intentional sampling was carried out. People with FM were recruited on social networks (Twitter®, Instagram®, Facebook®, LinkedIn®) on accounts dedicated to the project (@fibrojourney_) and through key informants (influencers in patient associations or networks, or doctors who suggested participation to patients they care for).
Health professionals were also partly recruited through social networks and also through key informants (in this case the coordinators of an FM training project were used). The latter selected and invited key people in their respective countries who usually deal with patients with FM.
For the patient groups, we tried to ensure that there were at least 6 per country, at least one male per country and not all from patient associations, with at least one per country of recent diagnosis and of varied age groups. Regarding clinicians, the indications for selection were that they be any health professional in the proportion in which they usually treat FM in their country (e.g., rheumatologists, primary care physicians, psychiatrists, psychologists, sports doctors, rehabilitators, pain doctors, etc.), regardless of years of experience and with geographic and gender variability. In both cases they were adults.
They were contacted by email or previous direct messages on social networks. Participation was in all cases voluntary, the study was carried out in accordance with the basic ethical principles contained in the Declaration of Helsinki and the good clinical practice guidelines, and data protection was maintained at all times. The protocol, informed consents and other study documentation were sent to an accredited independent committee for evaluation and, after reviewing the documentation, the committee agreed that since it is not considered a medical research study itself, as designed (i.e., a qualitative study), a drug research ethics committee does not evaluate this type of study.
Focus groups and dataNine focus groups were conducted, of which 3 were with people with FM and 6 were with health professionals. The groups lasted 1.5 h and were virtual (using the Zoom® platform), so that each participant was in a different environment, but familiar to each of them. They were moderated by non-practicing rheumatologist methodologists, with no prior relationship with the patients or professionals included (TO and LC), except in the case of a key informant with whom one of them had participated in studies on other topics in the past. Both are doctors and have experience in qualitative methodology. Only the moderators and participants were present.
The participants had previously attended a meeting to launch the study in which the methodology to be followed and the objectives were presented, together with an expression of the interest in knowing the experience of people with FM in Latin America and helping to develop action plans. In no case was there any commercial motivation. Both researchers maintained an empathetic and open attitude towards people who have FM and those who see patients with FM.
The variables were not predetermined, except for the descriptive ones, which in the group of patients were age, sex and duration of FM and in the group of health professionals the profession and years of experience.
Guideline questions were designed to be used by the moderators of the focus groups, which included open questions such as: what happened? How many health professionals or others were visited before finding a diagnosis? What was the diagnosis like? Who did the monitoring and how was it performed? Open questions were also used regarding problems in the relationship with the system, given that this was the structure used to collect information on maps of the journey. All groups were recorded (audio and video), with prior consent from the attendees for later transcription. TO and LC were responsible for transcribing the files including pertinent observations of the participants' mood, not just the speech. The transcriptions were checked between the 2 methodologists plus the graphic designer. The graphic designer also took notes from the recordings to specifically complete the maps of the patient journey.
AnalysisA methodologist (TO) used the Atlas.Ti© program for coding and synthesis with an inductive mixed technique (based on the points necessary for the journey map: actors, relationships and interdependencies, events, points of contact, emotions and obstacles /opportunities) and deductive technique (based on the themes and sub-themes that emerged in the focus groups). Furthermore, the graphic designer (MP) used the perspective of the user experience or patient-journey18–20 directly on the recordings, identifying actors, relationships and interdependencies, events, points of contact, emotions and obstacles and opportunities. Both analyses were carried out independently and were subsequently shared and discussed among themselves and with the groups from each country.
The results were prepared in the form of figures, trees and example verbatim, as well as journey maps. The creation of these maps was made by the graphic designer (MP), specialised in user experience (Ux).
ResultsParticipantsA total of 43 people participated, of which 33 were clinicians and 10 patients (of which 2 were men). This represents 53% of all those invited to participate (Fig. 1). Non-participation in the cases that responded was due to the difficulty in having a meeting at the agreed times. The participation rate was somewhat higher among health professionals than among patients (58% and 42%, respectively). The clinicians were mostly rheumatologists (n = 12 rheumatologists + 8 rheumatologists and internists + a clinical doctor and rheumatologist). There were also 2 family doctors, 2 physiatrists (one was also a general practitioner), a traumatologist, a rheumatologist paediatrician and a paediatrician, 2 anaesthesiologists/algologists (who were also palliative care), an internist, a physical activity and sports doctor and an emergency services doctor. By country, the participation rate was highest in Mexico (81%), followed by Colombia (43%) and Argentina (36%). The years of experience of the healthcare professionals ranged from one to 49.
Given the low patient participation, it was decided to also collect information from social networks and a forum prepared on a project website to which everyone had access. The information that was collected from these sources was not substantially different in content from that already collected and analysed. The information collected in the third group from each country added little information to that previously collected (saturation), so the moderators tried to guide the discussions towards collateral phenomena, including emotions.
Map of agents and interactionsFig. 2 shows the first result of the patient-journey: the map of agents and interactions. This can be divided into 3 spheres: health care, support and work life, and the socioeconomic context. In the sphere of health care, attention is drawn to the multitude of professionals who interact with these patients, both before and after diagnosis. In the sphere closest to the patient would be family and work. Specifically in the latter, interaction with the employer is important. In this sphere, together with that of health care, there would be patient associations. Finally, the socioeconomic context, with the government and active policies, will determine access to public or private healthcare, and the work policies that will determine whether a person with FM is covered during periods of greatest pain or fatigue or, if necessary, whether they can apply for disability allowances.
Map of the journeyFig. 3 shows the journey of the patient with FM. The journey line features 2 large sections, 2 loops and a thin dashed line. The 2 large sections represent the journey that starts from the initial symptoms to the visit to the doctor and the journey from diagnosis to follow-up. In the first, the patient has been feeling pain and other symptoms for several months that affect their daily life. They self-medicate with painkillers to alleviate the symptoms and, normally they do not go to the doctor, but talk to family members, neighbours and even "witchdoctors" who give them advice for treating their symptoms ("you self-medicate until it's worrying"). The emotion assigned to this phase is confusion and denial. After this stage, the patient decides to ask for help and enters a loop phase in which erroneous diagnoses and treatments occur, and referrals to specialists. In all cases the clinical tests are normal and distrust begins towards the doctors because they do not believe that the pain is real and they prescribe treatments that do not help, they do not know how to cure. The patient attends medical consultation without much hope, not expecting help but keeps on trying. They take the medication prescribed for the diagnoses given and nothing alleviates their symptoms. The emotion assigned to this phase is frustration, uncertainty and isolation ("I must be crazy because I have nothing"). This loop can continue for years, until the specialist visited knows how to diagnose fibromyalgia. At this point the other long leg of the journey begins. The patient is not usually aware of the disease and still does not understand why it has taken so long to diagnose it, but finally they have a diagnosis. They now think that they know what they have, they will be cured with treatment and will soon be able to live life normally again, which reassures them, although they doubt the certainty of the diagnosis ("They told me that what I had was an incurable disease”). They do not find enough resources about the illness and feel that doctors do not explain anything to them about fibromyalgia. The emotion of this phase would be relief, distrust, and hope. During this period, they also begin one pharmacological treatment after another, in which excessive expectations are raised, and generally with many adverse effects. They do not tolerate physical therapy well and refuse to go to a psychologist or psychiatrist. All of this leads to little trust in the doctors and their decisions ("they had to take too many drugs, they couldn't do anything alone"). The medication prescribed is increasingly more expensive and difficult to obtain. They begin to seek alternative therapies, if not already using them. They try to do the physical activities prescribed, but sometimes there are obstacles in the system. The emotion assigned to this phase is rejection, frustration and distrust. Here they also investigate the disease and discover the Associations, which they can turn to or not. Work adaptation also takes place. One cannot work under normal conditions, needing to adapt the job or stop working, but neither the employer nor the administration understands FM, which generates insecurity, frustration and sadness ("in the workplace there is no understanding"). They enter a new loop characterised by new symptoms every so often. They visit different specialists depending on the symptoms, and find themselves in situations that make them doubt their diagnosis.
Sometimes they need to spend a lot of time in the doctor’s surgery to let off steam. They are not always able to resolve all their doubts there. They search for another illness because they think they have a serious illness, not FM, and they distrust the treatment and diagnosis. Doubts and impatience arise ("it's a difficult cross to bear"). Very few patients manage to reach the final phase of autonomy. This is the moment in which the patient discovers that a high degree of self-management results in better coexistence with the disease. The patient adheres to treatment (pharmacological and non-pharmacological) and makes the necessary changes to their lifestyle. They manage to improve their symptoms and control outbreaks. They need to go to the doctor less, and the consultations are more satisfactory, making them feel hopeful ("therapy helps me accept that I am different"). This autonomy is the closest thing to a “goal” in FM, but not many patients achieve it.
The parallel part of the journey that the other agents are on is developed in the supplementary material. The family context can be very hard for these patients. The different specialists also feel frustrated in what they do, from lack of knowledge of the disease and its management, lack of time or patient confidence in non-pharmacological therapies, or lack of resources to appropriately refer to professionals who know and can treat the FM. Patient associations make up for many of the system's deficiencies.
Themes and sub-themesWe have divided the topics into 2 different moments, depending on whether they refer to the diagnosis or the management and follow-up of these patients.
DiagnosisWhen making the diagnosis, the groups highlighted the broad variety of symptoms that these patients can present as one of the great obstacles to obtaining a diagnosis. Both the professionals and the patients with the disease involved in the groups discussed different aspects to evaluate when making the diagnosis (aspects of FM itself and the system, to take into account). Also, the difficulties when making the diagnosis in different patients and the strategies involved (Table 1).
Themes and sub-themes with verbatim.
| Diagnosis | ||
|---|---|---|
| Symptoms | “eminently clinical""chronicity of pain""when the answer is everything""we didn't find anything inflammatory""unexplained pain, very intense which immensely complicates their quality of life”“Yes, the examination, listening to the patient, obviously the questioning. And sometimes, simply by questioning, from the type of pain, the characteristics that accompany it, in the limitations in their daily life, in sports activities, in their social relationships, etc., we already have an obvious clue that we are up against a condition of fibromyalgia, so yes, I also request laboratory tests to confirm that everything is in order” | “One has a very extensive journey to search for that diagnosis."“What I am sharing with you, it was almost 2 years from 2008 to 2010, until I was diagnosed with fibromyalgia”“I was diagnosed approximately 3 years ago, but I had different symptoms for about 15 years before that” |
| Aspects to assess in the diagnosis | “Affective and social factors and evaluating certain employment components”"acute stressful event"“risk of over diagnosing patients”"I receive them after more than 5−8 years of going around without diagnosis""They come with the need to be examined, to be touched, they perhaps have gone through many specialties where they have only been asked for reports and the patients have never been touched"“An initial psychological evaluation, if possible, because from the moment you tell the patient this has to do with mood disorders and the way one perceives and acts towards life and life's problems, this seems to them like something they generally reject.“They have been through 6 or 7 doctors before coming to you"“Patients with FM have a wide variety of symptoms, and also, there are some that have more emotional content, others more physical content, in short, you can find small subgroups within the FM patients themselves” | |
| Difficulties in the diagnosis | ”Fibromyalgia not only has a physical environment, but also an emotional environment and even a family environment sometimes”“I receive patients who have been without a diagnosis for a long time, and having travelled through the state system and the private system with different specialties and polymedication” “patients who have gone through all the tests, patients who come polymedicated, with high doses of pregabalin or duloxetine, with analgesics, with tramadol, with everything, with loads of tests, because they have already gone to the traumatologist, to rheumatologists, who did not resolve it, So they come for consultations. It also happens to me with patients who have not been for tests and who come with a diagnosis of FM, because some doctor told them it was FM and it wasn't. When I started doing all the tests it turned out that it wasn't FM, so for me, I always tell them that the most important thing for me is the difference in the diagnosis of FM and that this symptom of chronic pain is covering up a different illness underneath, because in oncology I sometimes see diagnoses of FM in oncology patients with other types of symptoms in which the diagnosis was not reached."“The lack of knowledge at high level is a barrier”“Tell the patient what they have”"I talk to them about the reality of the disease, about the quality of life they will have, which will depend on many factors but fundamentally on the patient." | “I think there is still a tremendous amount of misinformation”“to the one who has recently been diagnosed or who has not yet been diagnosed, and if they are diagnosed, then they continue looking to see what they have because initially they did not get this diagnosis” |
| Strategies to be used | “tell them that you believe them that it hurts because there is a kind of feeling in the family that the person is inventing the pain, so as a secondary benefit to everyone, by paying attention to them or more attention to them you have to say that this disease really exists""because that reassures patients, it reduces their anxiety, as perhaps in the first consultation someone does not give them any medication or orders them to do a test of some sort, but giving a name to the pathology, at least in my experience, always reassures them"“a patient who must be approached in a multidisciplinary manner and who requires a significant group effort, team work, a group with sometimes a psychiatrist, a neurologist specialising in pain, a physiatrist. All this means that the approach has to be very multidisciplinary and that requires an effort on the part of the doctor” | “I think a key point would be having information, having communication between the different specialities” |
| Difficulties and problems in monitoring | ||
|---|---|---|
| Training | ”Since the general practitioner does not have the sufficient tools of knowledge, because they do not acquire them in an undergraduate degree, they end up skimming the surface of it”“the problem with this training is in undergraduate degree""they don't have enough knowledge to focus on it"“there’s a big gap there even in the training of specialists”“In most universities, in undergraduate studies, students do not have a rotation for physiatry, rheumatology, or orthopaedics, since it is a basically surgical rotation” “They consider that it is something that the patient is inventing, that it is something psychological, or as XX said, it is normal that they do not want to go to work or that they want to invent themselves" “Physical medicine physicians are not very well trained, not made aware of the subject”"Many doctors do not believe in the disease and patients arrive disappointed" | “Because you go to primary care and the primary care doctor lacks enough scope.""They didn't know where to go"“There are doctors here who tell you that it does not exist” |
| Management | “They ask for many tests that are irrelevant and delay the patient's diagnosis”“There are colleagues who do not like managing patients with fibromyalgia, and prefer to send them to another specialty, but in general we stay with them”"I prefer to see autoimmune patients and I refer this patient to the rehabilitator, pain doctor or sports specialist"“A patient who has been going around the system, if someone gives them a diagnosis, do they calm down knowing it is fibromyalgia? Are they always looking for something else?“when you have the support of services such as clinical psychology, and that type of thing, you can rely a little more on that, but in the public hospital the management tends to be pharmacological, with very little time, and the success rate is not as good as at a private level, that's where things change."“I believe that patients with FM must be convinced that they should take their treatment for a few weeks and not a few days, because patients often believe that we are magicians, so we must ask them to adhere to the treatment for weeks and they will see an improvement”“It is difficult for us to assemble multidisciplinary teams""Patients more frequently suffer side effects from all the medication we give them and they tolerate very little, no matter how much we use small doses and try to combine all the drugs in the most rational way possible, they get side effects."“We do not properly assume that there is a whole range of things that have to be done in addition to medicine that is not so wonderful, it helps, of course it is super important, but disease is disease""They can't get the next consultation and they don't have anyone to write the prescription, so there they also lose adherence or continuity of treatment" | Some specialists say to the patients “I don’t treat fibromyalgia, don’t come to me”“I have already been to many specialists, I do not want to go to any more”“I have a diagnosis but I am still doing tests, I am still doing (…) this is a professional lack of understanding” |
| Other professionals | “Let it be the nurse who does the work, apart from recognising the patient's symptoms and so on, she can also collaborate in issues like education, because the nurse as such also has extensive knowledge of many things that could be used, which in general terms we do not do”"I believe that the area of nursing is a terribly underutilised area in our country""The role of the doctor is very important, and the assistance that nursing could provide is wrongly underestimated"“And trained nurses tend to become specialists. The specialist nurses who basically work in critical care, or in neonatal care"“Where not only the doctor participates in their role but where the nurse plays her part in her nursing role, and also as an educator, and a social worker, clinical psychologist and thanatologist” | “I began to have problems of that type and I searched for psychological help. And this was when I found my psychologist, XX who helped me a great deal, in the sense that I found out a lot of things and also I started to go out”. |
| Family and social environment | ”A serious level of family dysfunction”“This is a serious gap because there are actually few fibromyalgia patient associations, aren’t there?”“This invisibility of the problem, this thing that people do not look sick, and yet they cannot get out of bed because this label falls on them: hypochondriacs, malingerers, exaggerated, you want to ruin our lives, because it is also very fluctuating, both pain and fatigue, so it can be very limiting, they had a plan for the weekend and in the end, they don't go because they felt very bad, so it already seems like a purposeful issue and there begins to be a lot of family friction and finally the indifference of the doctors, which was also already mentioned”“some patients want quick and easy solutions. That is a problem”“It impacts the family economy”“There are patients who accept the illness and unfortunately I have had patients who sometimes go to initial consultations accompanied maybe by their husband and I don’t know, in the second or third consultation they have been abandoned, they are going through a divorce, because they finally decide not to accompany the patient with fibromyalgia and they forget that there are negative aspects”“There is no support network in the family and finally sometimes they have to continue alone and they do not always have an appropriate possibility of working”“The psycho-social economic issues mean that they even leave the rheumatology department because they do not have a family support network”“They are labelled weak, people simply do not understand” | “It’s difficult when you have a family that does not believe in the illness and they think it is nerves, that it is a psychological problem”“It took a long time for people to believe me”“How can you have that, you look very well to me.”“We are labelled anxious”“One's social life ends. I can't play sports, I don't go to meetings, I don't leave my house. "I can lift nothing, because if I do some work, I can't stand the pain.""Psychological help helped me (…) inside my house, which was also a very difficult situation because neither my husband nor my children understood me"“I rely on my wife and my son and they helped me a lot. But people are not seen… there are people who are already defeated and feel hindered by that”.”I try to get up every day and find a meaning to my life, but…some tell me that, on the street, life is no longer going at all for them."“Me, well, since I was diagnosed I have continued with the rheumatologist and I have been taking psychological therapy at the Crecer association. We use it online because, well, it was during the pandemic. And that has helped me a lot, first to know the disease, to understand myself, to analyse the situation and to assert myself”.“That, yes, I recognise now that I am different and that I have to accept myself and that is what the association, the therapies have helped me to accept myself, to love myself, to live with this new condition” |
| Autonomy | “There are patients especially, in my opinion, over 50 years old who do not know what to do with autonomy""They are accustomed to the paternalistic model and it is difficult for them to adopt new strategies, that is, it is an extra job that you have to convince them that it also depends on them, so it is complicated""Convincing them of the importance of practicing exercises and having a routine is complicated but has good long-term results"“Experience is invaluable to understand that holding patients responsible is truly complex, but I believe that this is the wonderful change of leaving paternalism and using autonomy”“I have noticed, and I will clarify, not only in fibromyalgia but also in general in chronic pain, I do notice a generation gap. It means, for example, that the patient's autonomy has been very valuable for them to participate in decisions and also respect it."“Make them see that it is a problem in which they are active participants, that it can become more chronic in some cases, perhaps in others it does not present as much of a problem and they respond better, but that there is no single solution, there are no magic solutions, and that it is important that patients are participants in the process""So that also influences therapeutic success, to what extent the patient is committed to being able to do things that improve his or her situation overall”“That obligation for them to take responsibility, to understand what is happening to them”“Ask them what they know about their disease or what they have been told, because, unfortunately, I have found that many times, rheumatologist colleagues and other specialists tell the patient that it is an incapacitating or disabling disease that is going to lead to a terrible quality of life prognosis and then I explain to them that this is not the case, that goals must be established according to their concerns and other times, perhaps, with multidisciplinary management."It takes a lot of work for the patient to really adhere to a pharmacological and a non-pharmacological therapy" |
FM: Fibromyalgia.
From the ideas transmitted by professionals and patients with the disease, it is during follow-up and continuous evaluation of FM that multiple obstacles appear. Perhaps the most shared by the participants from the 3 countries is the lack of adequate professional training, from undergraduate to specialisation. Also, different aspects of FM management and the active participation of other professionals, the need to also address the patient's environment and surroundings, as well as to encourage the patient's own autonomy (Table 1).
As a last point, we would like to highlight the shadow of "doubt" that arises in almost all diagnoses, from the beginning of the symptoms, to diagnosis and follow-up, arising from the environment, the professionals who care for people with FM, the work environment and the health system itself. In Table 2 we summarise that feeling of uncertainty that surrounds this disease throughout the process.
Verbatim expressing uncertainty.
| Professionals | Patients |
|---|---|
| ”They asked everyone and nobody gave them a solution, nor any type of medication that helped them to improve”“The doctors try to get rid of patients with FM” | “They gave me medication that did not resolve the problem nor reveal what I had”“The truth is that they treat us like third-.hand patients. Not even second, third. And you go to any specialist, any area of medicine, wherever you go…”“And it turns out that they classified me as suffering from depression, but they never mentioned anything about fibromyalgia” |
| “Enormous amounts of tests that include MRIs, ultrasounds, different types of tests and in general, almost everything is normal and the doctors try to get out of the consultation by asking for new studies that are usually normal and the patient comes saying everything hurts, they say "I have nothing but everything hurts me""I have already tried everything, what are you going to give me?" | |
| “The anaesthesiologist told me 'yours is a problem of the mind'. I felt offended but the fact is that I told him…""Why is this happening to me if I have nothing?""Do you actually feel disabled?" | |
| “If you see fibromyalgia you are not a rheumatologist” (contempt for the professional who sees FM) |
FM: fibromyalgia.
In our study we have verified how access barriers in the system lead to self-medication, postponing the medical visit and consequently the diagnosis and treatment. Likewise, the general lack of knowledge about the disease and the rejection of its existence delays the diagnosis more than necessary.
Patients with FM report difficult experiences with the healthcare system.11,21,22 It is common for them to feel disappointed, ignored or helpless during the relationship they establish with health professionals and the system.11,23–25
We have also verified that, once FM is diagnosed, patient education is essential for adherence to treatment, but rarely is the person who makes the diagnosis also capable of offering adequate education. The diagnosis is received if the patient is "lucky", if they find a doctor who knows about the disease. This means for the patient that they have to go around the system until a doctor knows about FM and diagnoses it. Not having unified clinical records and offering such fragmented care creates obstacles not only in obtaining a diagnosis, but also makes its validity and treatment difficult among different specialties.
Participation in healthcare support can also be difficult due to obstacles to accessing specialised medical consultations.26,27 Several studies have focused on the doubt and anguish of patients who do not perceive adequate medical care, as well as their search for legitimacy and their resistance to psychological explanations of pain and suffering.28–31 Nomadism and patient stigmatisation, as well as the ambiguities and difficulties of doctor/patient interaction, have also been widely investigated.32–40
Participants recognised that the most effective treatment for FM is multimodal, but both system barriers and patient reluctance complicate adherence. Adherence to treatment is not good and when improvement is noted, treatment is abandoned.
Hayes et al., report the feeling of helplessness experienced by doctors facing FM.11 This context of dissatisfaction and questioning of mutual trust can, as Durif-Bruckert et al. demonstrate, amplify pain.41 The search for treatment is then concomitant with the search for a relationship based on mutual trust and good will. Another study also pointed out that a medical prescription can be a sign “of the doctor's interest and the right to access therapy”.42
Another finding of the study is that work helps many patients feel useful and stay busy. The goal should not be to seek disability. However, although maintaining work is beneficial for patients, it is not always possible due to the characteristics and limitations of each job. Therefore, being able to receive disability is economically necessary for many patients. FM is a negative diagnosis, both for doctors and employers.
The lack of consensus among different professionals to accept the diagnosis aggravates the uncertainty and general situation of the patients. If the patient is fully aware of their FM, they are capable of self-management and will be able to make appropriate decisions independent of the opinions of professionals who do not believe in the existence of the disease. FM can get better or worse at different points in life, but it is still a chronic disease. Based on what was commented on by the participants, autonomy can be very useful for symptomatic control.
When presenting the results to the groups by country, we asked them to try to identify priority problems and propose solutions. In general, everyone insisted on improving training, both of specially related doctors, including generalists, and of other health professionals involved (psychologists, physiotherapists, etc.) and even expert patients (at the university, in associations [p. e.g., ACED]), by the industry, by insurers (refresher courses). The need to increase knowledge and dissemination of the disease was also insisted on, based on information and dialogue with the patient and their environment to reduce the stigma of FM. The information offered must be truthful, objective, up-to-date, and it must be well understood that this is a disease that cannot be objectified, but that has its impact, and that the stigma on mental health should be removed. Regarding channels, the collaboration between patient and professional associations (conferences, websites, development of materials), institutional channels such as TV or campaigns stood out. Both patients and professionals need to improve the knowledge and training of patients with FM. To this end, it is proposed to use explanatory/educational brochures in medical waiting rooms, take advantage of all existing resources, especially those developed by patient associations, as educational material for patients (on healthy habits, physical activity, self-care, self-assessment, self-control and self-management). Regarding the needs at the health system level, it is critical to make the “this disease is yours or mine” disappear: FM can be evaluated and treated by different medical and non-medical specialists. Furthermore, it is proposed to define the cost of the disease for the system and demonstrate that comprehensive FM services are cost-effective for the system. Finally, an individualised assessment of disability must be made, not based on having or not having a specific illness, for which measures to fight for rights are proposed.
As this is a qualitative study, there is no possibility of making measurements, and certain sections of the results obtained may not be extrapolated to all patients (due to possible difficulty in data analysis or problems when selecting patients included). An attempt was made to ensure that the patients and professionals were highly representative, and to cover all spectrums of FM involvement, so as not to lose information. It is worth considering that despite having attempted to make a representative selection, there may be a bias with the choice of participating clinicians, since the health personnel in contact with these patients have a different way of seeing and treating them, unlike those who prefer not to see them and therefore do not participate in this type of studies.
In conclusion, we can say that the journey of a person with FM in Latin America is far from simple and is full of obstacles and loops, but that it is possible to identify a way out if all the agents involved understand that self-management, the desired goal, can only be achieved with access to resources in an early and professional manner.
FundingFibrojourney was financed with funds from the Musculoskeletal Health Institute, S.L., in collaboration with Viatris.
Conflict of interestsTO and LC did not receive personal fees or grants from any laboratory, but their institute works under contract for laboratories among other institutions such as Amgen, Fresenius Kabi España, Galapagos, Gilead, Pfizer, Lilly, Meda Pharma, MSD, Novartis, Roche, Sanofi Aventis, Upjohn, BMS, Novo Nordisk and Sandoz.
ODM has received fees from Lilly, Pfizer and Amgen.
DGFA, MRSR, AC and CA declare the absence of conflict of interest.
We would like to thank Victoria Romero Pazos, from Triple Axel, for her diligent communication with the participants and social networks, and to Esther Martín-Blas, who prepared the Inmusc campus where the Fibrojourney project could be included and was in charge of the logistics. Likewise, we thank Estíbaliz Loza for her participation in the final discussion group as moderator.
Argentina: Osvaldo Daniel Messina, Andrea Carvallo, Constanza Arguissain, Agustina Cáceres, Antonio Catalán Pellet, Beatriz Rodriguez, Dario O Mata, Eduardo Mario Kerzberg, Eliana Blanco, Jorge David Pujol, Juan José Scali, Lidia Cazal, Marina Soledad Dalpiaz, Mercedes Rodriguez, Miriam Mainieri, Mónica Meinardi, Norma Garrone, Norma Galasso, Ofelia Rivas, Pablo Beretta, Sabrina Martini, Soledad Andersen, Tomás Maresca, Verónica Garro and Zulema Costas.
Colombia: Daniel Gerardo Fernández Ávila, Julián Barahona, Ana María Arredondo, Andrés Garzón Forero, Ángela Maryoure Gigliola Suárez Moya, Angie Guasca, Annie Girón, Carlo Vinicio Caballero, Carlos Arteaga, Carlos Enrique Toro, Catalina Villota Eraso, Diana Gil Calderón, Bertilda Bernal, Eduardo Muñoz Jiménez, Francy Nelly Pérez Becerra, Jenny Paola Varela Rojas, Gina Ochoa Galeano, Josefina (Pepita) Bernat de Hurtado, Liliana Carolina Mancipe, María Lucía León, Monique Chalem, Olga Marcela Andrade Salazar, Oscar Virguez, Oscar Ruiz, Sonia Canchón, Sandra Navas, Susana López, Wilson Bautista-Molano, Yudy Milena Rodríguez Mojica and Guillermo Alfonso López.
Mexico: Manuel Robles San Román, Alejandro Maya Gutierrez, Argelia Lara Solares, Blanca Adela Mota Mondragón, Cristina Hernández Díaz, Daniel Xibille, Emi González Martínez, Fedra Irazoque Palazuelos, Felisa Crespo Campos, Francisco Javier Silva Lira, Georgina Domínguez Ocadio, Ivon Karina Ruiz López, Jorge Miguel Galindo Guzmán, Juan Carlos Cajigas Melgoza, Lilia Andrade Ortega, Lucio Ventura Ríos, Margarita Eugenia Araujo Navarrete, María Morales Lopez, Maria Eugenia Dávalos, Maricruz Ríos Medina, Miriam Martinez Arriaga, Norberta Cruz Ortiz, Patricia Clark, Rodrigo Sánchez Rowold, Samara Mendieta Cerón and Teresa Oviedo Lugo.