We present the case of a 35-year-old Caucasian male with a history of mechanical low back pain for a year that had improved with NSAIDs. He came to the emergency room due to swelling of the left lumbar region, which had appeared two months prior associated with important pain. Fifteen days earlier he had high fever and a runny nose, labeled as a respiratory tract infection and treated with azithromycin with complete resolution of this process.
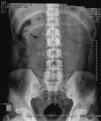
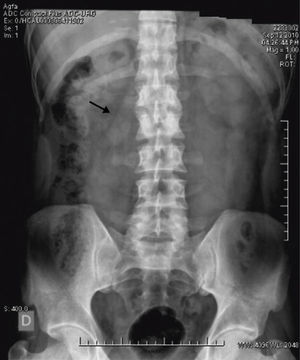
In the ER, he underwent a blood count, coagulation tests, glucose, urea, creatinine, ions, liver function, lipid and kidney laboratory determinations within normal results. We found no elevated acute phase reactants and nutritional parameters were within normal limits. The abdominal X-ray showed effacement of the left psoas (Fig. 1).
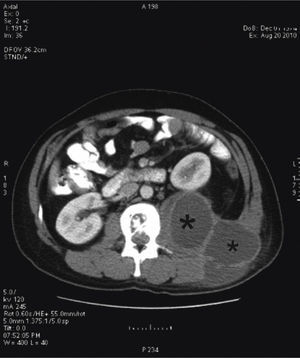
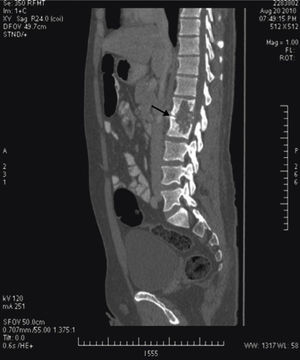
We then requested a CT that found a lytic lesion with a sclerotic rim in the L1 and L2 vertebral bodies, centered on the disc, compatible with spondylodiskitis. It was accompanied by a large abscess of the left psoas and lumbar musculature, which pushed the left kidney forward and extended to the subcutaneous tissue (Figs. 2 and 3). A CT-guided puncture allowed us to withdraw 440cm3 of purulent fluid. The smear found 10bacilli/field and the culture grew Mycobacterium tuberculosis.
The patient was treated with drainage of the abscess and four anti-TB drugs (rifampicin, isoniazid, pyrazinamide and ethambutol) for 2 months and then continued treatment with three drugs (rifampicin, isoniazid and pyrazinamide) for another 10 months until resolution of the problem, with a control study with X-rays and abdominal CT of the spine showing complete disappearance of the abscess. He is currently without clinical complications 6 months after completing treatment.
DiscussionOsteoarticular TB is the third most common variety of extrapulmonary tuberculosis, accounting for 1%–5% of the total, and with a greater axial involvement, which may be present in 71%,1,2 producing the condition known as Mycobacterium tuberculosis tuberculous spondylodiskitis. The delay in diagnosis due to the nonspecific clinical features may take several months,3 plus it is able to simulate other pathologies (brucella, neoplastic, etc.), although the presence of low back pain with low grade fever, normal acute phase reactants and an elevated ESR most likely suggest a tubercular etiology when there is lack of other microbiological data.4 Simple X-rays take more than 8 weeks to show bony involvement,5 with CT or MRI being more specific for the diagnosis. Its progression may be associated to a cold abscess (12%), fistula (9.4%) or affect nearby structures, such as the psoas or neurological tissues (spinal cord compression in 9.4% of cases),2 producing what is called Pott's disease6 or abscess, hindering treatment. A surgical approach is necessary in a third of patients,2 although this case was solved with medical treatment.
The interest of this case lies in the presentation and nonspecific clinical presentation despite the remarkable involvement seen in the CT images. It also demonstrates the usefulness of this diagnostic study in order to achieve early treatment, and to demonstrate an involvement as remarkable as the one seen in the image.
Ethical disclosuresProtection of human and animal subjects. The authors declare that no experiments were performed on humans or animals for this investigation.
Confidentiality of Data. The authors declare that they have followed the protocols of their work centre on the publication of patient data and that all the patients included in the study have received sufficient information and have given their informed consent in writing to participate in that study.
Right to privacy and informed consent. The authors have obtained the informed consent of the patients and /or subjects mentioned in the article. The author for correspondence is in possession of this document.
Please, cite this article as: López-Sánchez MC, et al. Espondilodiscitis tuberculosa con tumoración lumbar. Reumatol Clin. 2012. doi:10.1016/j.reuma.2011.10.011