Polyarteritis nodosa (PAN) is a rare form of vasculitis which involves medium and small sized arteries. It can involve any system of the body, but lungs are typically spared. PAN typically presents with non-specific symptoms, such as fever, weight loss and myalgias, and symptoms related to the system involved. Negative serum ANCA helps in differentiating it from other similarly presenting vasculitis and definitive diagnosis is made on histopathology. Limb ischaemia is a rare presentation as well as a rare complication of PAN. We present the case of a 28-year-old female who presented with severe lower limb ischaemia and intermittent leg claudication as initial symptoms which led to initial diagnosis of critical limb ischaemia. Later in the course of the illness she developed gastrointestinal symptoms and weight loss. She was diagnosed as having PAN based on laboratory results and histopathological evidence. Intravenous steroids halted the progress of the disease, but the patient required transmetatarsal amputation of the foot to remove dead tissue. Vasculitis like PAN, although much rarer than atherosclerotic peripheral vascular disease (PVD), should be considered as a differential diagnosis in cases of limb ischaemia in which there is lack of risk factors for PVD.
La poliarteritis nudosa (PAN) es una forma rara de vasculitis que afecta a las arterias de mediano y pequeño calibre. Puede afectar a cualquier sistema del cuerpo, exceptuando los pulmones. La PAN cursa normalmente con síntomas no específicos tales como fiebre, pérdida de peso y mialgias, y los síntomas relacionados con el sistema afectado. Los ANCA séricos negativos ayudan a diferenciarla de otras vasculitis con presentación similar, realizándose el diagnóstico definitivo mediante histopatología. La isquemia de las extremidades es una presentación inusual y una complicación rara de la PAN. Presentamos el caso de una mujer de 28 años con isquemia en las piernas y claudicación intermitente de la pierna como síntomas iniciales, que condujo a un diagnóstico inicial de isquemia crítica de las extremidades. Posteriormente, en el curso de la enfermedad, desarrolló síntomas gastrointestinales y pérdida de peso. Se diagnosticó PAN, sobre la base de las pruebas de laboratorio y la evidencia histopatológica. La administración intravenosa de esteroides interrumpió el progreso de la enfermedad, pero la paciente precisó amputación transmetatarsiana del pie para eliminar el tejido muerto. Las vasculitis de tipo PAN, aunque son mucho más infrecuentes que la enfermedad vascular periférica (EVP), deberán considerarse como diagnóstico diferencial en los casos de isquemia de las extremidades, en las que no existieran factores de riesgo de EVP.
Polyarteritis nodosa (PAN), first described as periarteritis nodose by Kaussmal in 1866,1 is a rare form of vasculitis involving multiple organ systems in the body. Most commonly affected systems are skin, gut, and kidneys but it can involve any organ of the body typically sparing the lungs.2 Although Aetiology of the disease is not clear, association of some cases with HBV infection suggests autoimmune nature of the disease.3 PAN typically presents as cutaneous lesions, hypertension, abdominal pain and neurological manifestations like Mononeuritis multiplex on the background of chronic fatigue, myalgias and weight loss.3 The levels of acute phase reactants are usually elevated. Absence of serum ANCAs helps in differentiating PAN from other similarly presenting forms of vasculitides.3 A milder variant of the disease is cutaneous PAN which is limited to the skin presenting as subcutaneous nodules, livedo reticularis, and skin ulcers.4 Aneurysms and occlusive lesions of the medium sized arteries are the usual findings on the angiography and histopathology of the involved tissue reveals necrotizing vasculitis.2,3,5,6 Prognosis of untreated PAN is dismal with 5 years survival calculated to be as low as 13% in a study.5 Treatment with corticosteroids and immunosuppressants improves the outcome especially if taken early in the course of the disease.5 Intermittent claudication and limb ischaemia are very rare initial presentations of PAN and can lead to misdiagnosis of peripheral vascular disease, which is entirely different from PAN in aetiology, management and prognosis.7 We report a case of 28 years old female who presented with intermittent claudication and foot ischaemia as the main complaints which turned out to be PAN after thorough workup.
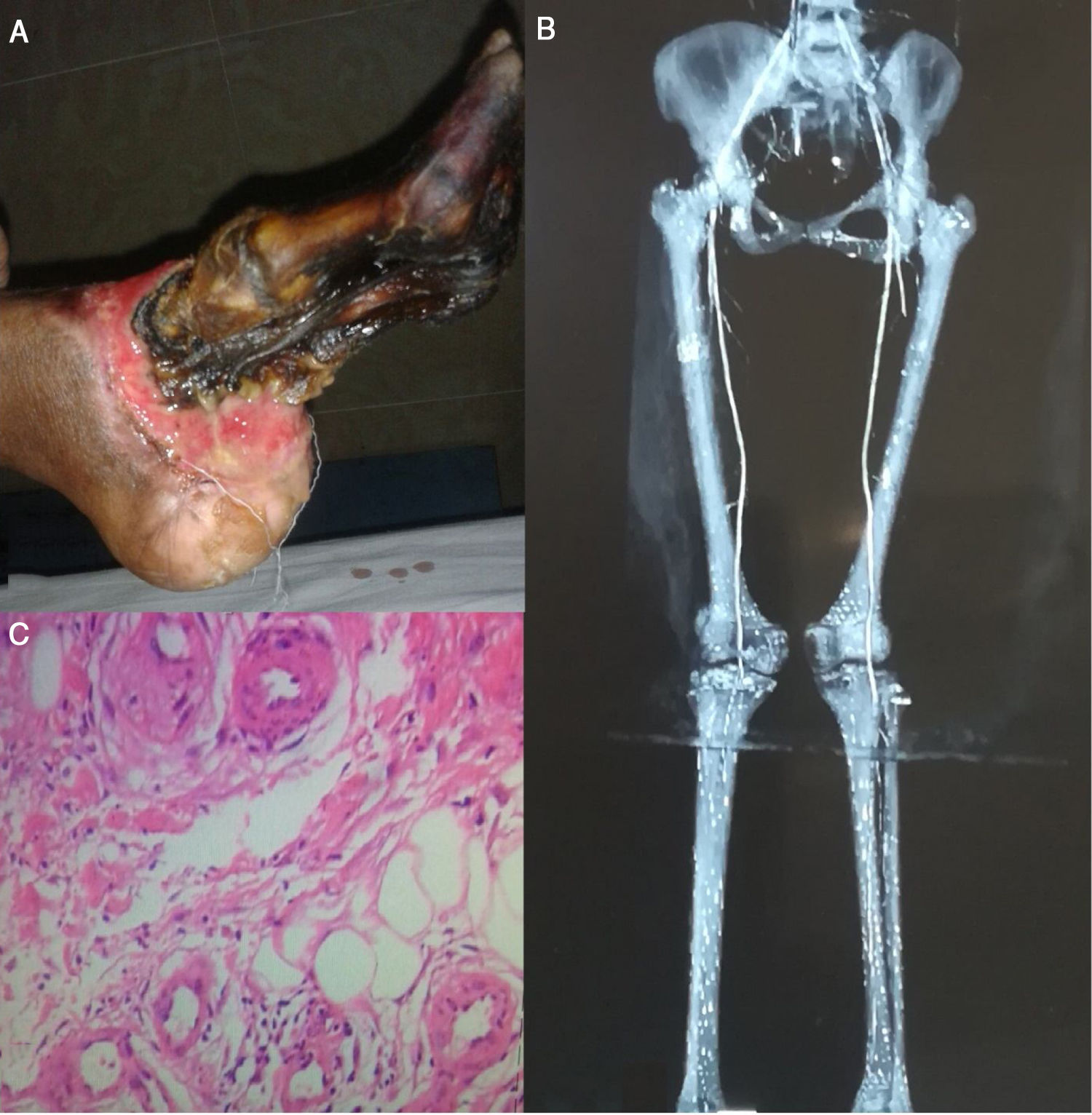
Case reportA 28 years old woman presented to our hospital because of progressive painful blackish discoloration of her left foot which started from the big toe and progressed up to the heel over a 4 months period (Fig. 1A) and was associated with intermittent claudication, on and off low-grade fever, blackening of the right first, second and third toe almost one month later,diffuse abdominal pain poorly relieved with medication and a weight loss of six kilograms during this period. The patient did not have any history of smoking, allergies, Raynaud's phenomenon or any similar complaints neither in the past nor anyone had them in the family. The patient had received anti-coagulants from local hospital but no beneficial effects were achieved. Pulse was regular, symmetrical and comparable in the upper limbs but absent in the lower limbs. In the left foot there were necrotic changes (dry gangrene) up to heel and in the right foot first three toes were involved up to MP joints. Rest of the examination was unremarkable. CBC showed Hb 9.8g/dL, WBC 13,200/uL, platelets 232,000/uL. Erythrocyte sedimentation rate was 44mm/h. Creatinine was 1.9mg/dL and urea was 48mg/dL. Liver function tests were within normal range. Alkaline phosphatase was 860U/L. HbsAg and anti-HCV were negative. Anti-Nuclear antibodies, anti-Cardiolipin antibodies IgM and IgG were normal (0.49, 4.36 and 5.26U/ml respectively). CXR, echocardiography and abdominal ultrasound were unremarkable. CT angiography showed multiple filling defects in the segmental branches of left renal artery with small left kidney, a filling defect in the distal 6cm of abdominal aorta extending upto both common iliac arteries and collateral flow was seen from superior mesenteric artery to external iliac artery. Filling defects were seen in left tibio peroneal trunk and in right distal femoral artery along with gradual attenuation of right anterior tibialis artery and absent dorsalis pedis (Fig. 1B). Diagnosis of PAN was made on the tissue diagnosis taken from the involved skin (Fig. 1C). The patient received iv steroids which improved the symptoms and halted the disease process but transmetatarsal amputation of left foot was done as dry gangrene converted into wet gangrene. At 6 months follow up the gangrenous changes in the right foot were conserved and patient had no symptoms of the active disease.
DiscussionPeripheral arterial disease (PAD) is a relatively common condition with its own risk factors, aetiology, treatment and prognosis.8 PAD is the first differential of limb ischaemia and intermittent claudication and it is very rare for PAD to be confused with vasculitis. In the literature there are few other reports of PAN unusually presenting as limb ischaemia although none of them required amputation.7,9,10 In our patient, although there was no risk factor for PAD, the initial complaint of pain and gangrene led to misdiagnosis of peripheral arterial disease (PAD) because there were no other features like renal, bowel, and nerve etc. involvement to suggest vasculitis. The patient also received a trial of anti-coagulants but no benefit was achieved. However, as the disease process progressed bowel and renal involvement became obvious which led to suspicion of systemic vasculitis. Arteriogram and biopsy revealed features suggesting PAN and the patient satisfied following 4 out of 10 points of American college of Rheumatology criteria for diagnosing PAN: weight loss >4kg, evidence of vasculitis on biopsy of small and medium sized vessels, elevated serum creatinine and arteriographic abnormalities.11 Although distal part of descending aorta was involved which is not usually involved in PAN, other evidences overwhelmed the possibility of any other diagnosis. IV steroids were started but by that time trans metatarsal amputation was inevitable as dry gangrene converted to wet gangrene. Apart from that patient's condition improved rapidly.
In a case of limb ischaemia when there is lack of risk factors and other features of PAD, there should be high degree of suspicion for PAN as reaching the correct diagnoses and starting early treatment are crucial for its prognosis.
Ethics approval and consent to participateThe study protocols and informed consent was taken with permission to use images investigations and all related material.
FundingThere is no role of any funding agency in this study.
Authors’ contributionsSarmad Zahoor: Initiated the idea. Participated in manuscript writing and diagnosing the disease.
Samara Siddique: Reviewed the article and Managed all investigations with follow-ups.
Hafiz Mudabbar Mahboob: Drafted the manuscript and followed up the patient.
Conflict of interestsThe authors declare that they have no competing interests.