We report the case of a 47-year-old man with a 9-year history of psoriatic arthritis (PsA) in whom we detected renal involvement, hypocomplementemia, peripheral neuropathy, acral necrotic lesions and positive cryoglobulins. The results of the diagnosis led us to conclude that the clinical picture corresponded to cryoglobulinemic vasculitis concomitant with PsA. In addition, we present a review of the literature on the presence of these two diseases in a single patient.
Se presenta el caso de un paciente de 47 años con antecedente de artritis psoriásica (AP) de 9 años de evolución en quien se encuentra compromiso renal, hipocomplementemia, neuropatía periférica, lesiones necróticas acrales y crioglobulinas positivas. Luego de realizar el abordaje diagnóstico se concluye que el cuadro clínico corresponde a una vasculitis crioglobulinémica concomitante a la AP. Se expone además del caso una revisión de la literatura referente a la presencia de estas 2 enfermedades en un solo paciente.
Cryoglobulinemic vasculitis has been associated with several clinical entities, chiefly with infections (especially hepatitis C virus, haematological neoplasms and autoimmune conditions.1 The presence of this type of vasculitis has rarely been described in cases of psoriasis or psoriatic arthritis.2 Treatment of this form of secondary vasculitis will aim to control the activity of the underlying disorder. If it is not associated with infection, treatment will be based on the use of high doses of steroids, cyclophosphamide, rituximab or plasmapheresis (depending on the severity of involvement of the affected organs).3 This paper present the case of a male with cryoglobulinemic vasculitis in the presence of previously diagnosed psoriatic arthritis; it also contains a review of the literature on the clinical and therapeutic approach in this unusual combination.
Clinical caseA male patient 47 years old with a history of psoriasis and symmetrical multiple joint psoriatic arthritis that had evolved during 9 years, with little out-patient monitoring and poor adherence to treatment. One month before admission he was examined as an outpatient by Rheumatology, which found the patient had high levels of activity in the skin and joints, so that the decision was taken to commence treatment with methotrexate, ustekinumab and medium doses of steroids. However, there was no continuity in formulation and the patient continued his treatment solely with steroids. He visited the Emergency department with clinical symptoms that had evolved over 4 months, characterised by paresthesia in both feet, a dropped right foot and progressive oedema of the lower limbs, as well as arthralgia in the wrists, metacarpophalangeal joints (MCP), knees and subjective weight loss.
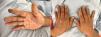
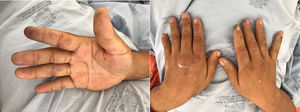
Physical examination found oedema of the lower limbs, restricted movements of the left wrist and the ankles, arthritis of the left wrist and knee, burst hands and pain in the second metacarpophalangeal joint of the same hand. There were common psoriasis lesions in the skin of the elbows and forearms, as well as small ischemic lesions in the fleshy parts of the fingers (Fig. 1). Neurologically there was bilateral hypoesthesia in the lower legs and a dropped right foot.
The paraclinical symptoms included a mild microcytic anaemia (Hb 10.7g/dl; VCM 79fl) with lymphopenia (380mm3), ferritine 264ng/ml and 16% transferrine saturation%; creatinine (Cr) 1.9mg/dl, giving calculated clearance of 28ml/min/1.73m2, urine analysis with proteinuria and soft sediment, 24 hr. proteinuria of 4,398mg with a urine volume of 2,620ml. Viral infection studies (HIV, HBV and HCV), as well as VDRL serology were negative. Biochemical inflammation was detected in the patient (PCR: 2.2mg/dl; VSG: 41mm/hr.). The decision was taken to request other studies to evaluate other non-infectious causes of his symptoms. These gave the results of negative rheumatoid factor, ANA, anti-DNA and ENA, but with hypocomplementemia (C3: 85; C4: 8,6). Nerve conduction electromyography of all 4 limbs showed sensory and motor axonal polyneuropathy in the lower limbs. Renal biopsy showed focal and segmentary glomerulosclerosis of the “TIP” type (involving the tubular pole) with acute tubulointerstitial nephritis and mild chronic changes.
Given the suspicion of vasculitis due to cutaneous, renal and peripheral nervous system involvement, ANCA were requested (using IFI and ELISA) and these were negative, although the report of blood cryoglobulins was positive. Due to the above findings a high probability of cryoglobulinemic vasculitis was considered, and it was decided to commence pulses of 250mg IV methylprednisolone every day for 3 days, initially improving kidney function and the joint symptoms. A subsequent medical meeting between nephrology and rheumatology decided to start treatment with rituximab (at a dose of 1g day 0 and 1g day 14) to control cutaneous vasculitic activity and joint and renal involvement.
The patient started to improve in kidney function and joint symptoms were controlled, as were the cutaneous vasculitic lesions, with no deterioration of the cutaneous domain affected by psoriasis. He was discharged with methotrexate, low doses of steroids and a new prescription to apply rituximab.
DiscussionCryoglobulins are circulating immunoglobulins that precipitate with cold (at temperatures below body temperature) and they become soluble again when the temperature increases.1
Cryoglobulinemia is confirmed by the detection of proteins that precipitate from patient serum when it is kept at 4°C during at least 7 days. The detection of cryoglobulins in the blood in the presence of symptoms suspicious of vasculitis such as palpable purpura, peripheral neuropathy and glomerulonephritis, leads to the diagnosis of cryoglobulinemic vasculitis.3
Classically, 3 types of cryoglobulinemia have been described: type I where there is a typically IgM monoclonal immunoglobulin associated with a B cell lymphoproliferative disorder, type II which consists of a polyclonal IgG with monoclonal IgM that has rheumatoid factor activity, and type III that is characterised by polyclonal IgG and IgM. The so-called mixed cryoglobulinemias (types II and III) have mainly been found to be associated with hepatitis C infection, connective tissue diseases and occasionally with haematological neoplasms.
In cryoglobulinemic vasculitis organ involvement derives from the formation and deposition of immunocomplexes on vessel walls.3
The relationship between cryoglobulinemic vasculitis and psoriatic arthritis has rarely been described in the literature. The most representative case is perhaps the one published in 2006 by Palazzi et al., who describe the case of a patient with psoriatic arthritis and purpuric lesions on the limbs, with a positive test for type III cryoglobulinemia. The symptoms improved with high doses of steroids and methotrexate.2
In the case presented in this paper, the presence of constitutional, neurological and cutaneous symptoms unexplained by the underlying disease was striking. Additionally, the findings of kidney involvement and hypocomplementemia indicated the presence of a secondary vasculitic process, caused by circulating cryoglobulins in this case which were persistently positive (2 measurements).
Respecting the kidney involvement, the patient had focal and segmentary glomerulosclerosis, a rare form of involvement given that the most common renal involvement described in cryoglobulinemic vasculitis, whether or not it is secondary to HCV infection, is membranoproliferative glomerulonephritis.4 It has mainly been observed in patients with mixed type II cryoglobulinemia in which the monoclonal component is IgM kappa, and its most frequent clinical manifestation is isolated proteinuria or haematuria.5 In spite of the above considerations, other forms of renal histological involvement have been described in association with cryoglobulinemic vasculitis. These include membranous GMN, nephropathy caused by IgA, post-infection GMN and focal and segmentary glomerulosclerosis.6
There was no evidence of pharmacological exposure, intercurrent infection or underlying neoplasm that would better explain the patient's symptoms, and everything pointed to the diagnosis of cryoglobulinemic vasculitis.
Treatment of this disease is based on the use of high doses of glucocorticoids, cytotoxic substances such as cyclophosphamide or rituximab, especially in severe manifestations of the disease, most especially those with neurological or renal involvement. One of the main references for the possibilities of treating patients with cryoglobulinemic vasculitis may well be Cryovac multicentre study with 242 patients, where the greatest benefit in terms of clinical, renal and immunological response (more than 50% reduction in basal creatinine and/or more than 50% increase in the serum level of C4) was obtained by combining rituximab with steroids.7 This combination is more effective than solely giving steroids. There are no clinical trials that compare rituximab with other agents such as cyclophosphamide head-to-head. Nevertheless, in scenarios where there is no infectious aetiology, cyclophosphamide may be considered a suitable alternative treatment.7 There are no conclusive data on the management of the association between psoriasis and cryoglobulinemic vasculitis due to the rarity of this combination. In 2010 Moberg et al. described a case of psoriasis associated with type II cryoglobulinemic vasculitis, where following a course of treatment with rituximab control of the cutaneous vasculitic lesions was achieved (with stability of the psoriasis lesions).8 In general the treatment for this specific association is extrapolated from recommendations for other causes of non-infectious cryoglobulinemic vasculitis.
Once the response had been achieved follow-up took place at approximately every 3 months, as relapses occur frequently with this entity.1
In the case of this patient, 9 months after starting treatment there has been no renal deterioration or relapse in the vasculitic lesions or joint symptoms. The neurological involvement was resolved, and repeated measurements of cryoglobulins have been negative. Nor has any deterioration in the common psoriasis lesions been detected.
ConclusionThe concomitance of cryoglobulinemic vasculitis in patients with psoriatic arthritis is unusual and anecdotal. In cases such as the one described herein, with predominantly renal, vasculitic cutaneous and neurological involvement predominated, rituximab was an available alternative for control of the disease.
Conflict of interestsThe authors have no conflict of interests to declare.
Please cite this article as: Urrea-Pineda LY, Gómez-Jiménez S, Jaramillo-Arroyave D, Muñoz-Vahos CH, Vanegas-García AL, Vasquéz G, et al. Vasculitis crioglobulinémica y artritis psoriásica: reporte de caso de una inusual asociación . https://doi.org/10.1016/j.reuma.2018.03.003