The presence of hypopigmented lesions on a patient is a diagnostic challenge. The causes of the lesions can vary, from the cutaneous manifestation of systemic diseases to local reactions to external agents.
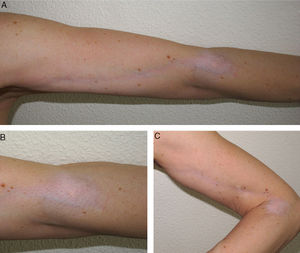
We present the case of a 53-year-old female that came to the consultation because of a hypopigmented, depressed skin patch of 2 months’ evolution on her left arm (Fig. 1). Relevant medical history included chronic migraine, idiopathic hyperprolactinemia and epicondylitis in both elbows. Her habitual treatment consisted of amitriptyline, paracetamol and also periodic intra-articular injections of triamcinolone in the 2 elbows—the last having been given 5 months before this consultation. The patient did not report any other relevant signs or symptoms. Examination revealed a hypopigmented atrophic skin patch on the left elbow that extended linearly along the inner side of the upper arm.
Cutaneous biopsy revealed atrophy of the epidermis. The dermis looked normal, without any associated sclerosis, changes in the adnexa or notable inflammatory infiltrates. No significant reduction was seen in the number of melanocytes.
Given the clinical–histological findings, the diagnosis was linear skin hypopigmentation and atrophy after intra-articular injection of triamcinolone acetonide. The patient presented progressive improvement of the lesion until its complete resolution was seen at 8 months of follow-up.
Intralesional injection of corticosteroids is very common in standard clinical practice.1–3 This practice concentrates more of the drug in the area with a better safety profile, avoiding some of the characteristic systemic side effects, such as iatrogenic Cushing syndrome and the suppression of the hypothalamic–pituitary axis.
Linear hypopigmentation following intralesional or intra-articular injection of corticoids has been described many times, usually associated with the use of triamcinolone acetonide.4 A similar condition was recently described in a patient with chronic foot eczema, who had applied a high-strength corticoid topically.5 In a series of 440 paediatric patients that were given intra-articular injections of triamcinolone acetonide or methylprednisolone acetate, slightly less than 2% of the patients later developed cutaneous hypopigmentation or atrophy in the injection area.6
The condition usually presents as an atrophic and hypopigmented skin patch with branching edges in the injection area; there is also linear extension of the lesion towards the perilesional area, normally following a pattern of lymphatic distribution. Differential diagnosis against other conditions such as linear morphea (localised scleroderma) or eosinophilic fasciitis should be considered, given the similarity in the clinical presentation of the condition that is described here.
This condition manifests after a variable length of time, which can range from weeks to months, following the injection. It can appear after either a single injection or following multiple injections, above all if quantities more than 10mg/ml are injected.
Skin atrophy from corticosteroids is due to their anti-proliferative effect on fibroblasts and keratinocytes, as well as from alterations in lipid synthesis and in the metabolism of extracellular matrix proteins. The mechanism behind hypopigmentation is less known; it might be due to an alteration in melanocyte secretion, without totally destroying the melanocytes.3
The linear extension that is a feature of this condition probably stems from dispersion through the lymphatic system. Kikuchi and Horikawa7 demonstrated this distribution after injecting colouring agents such as blue dye in the initial site of the lesion and confirming its later extension through the lymph vessels.
There is no specific treatment. However, avoiding new injections is generally recommended. It usually takes months after condition onset for the hypopigmentation to disappear and the skin atrophy to improve.
We would like to thank Dr. Verónica Parra Blanco for the histopathological study.
Please cite this article as: Hernández Aragüés I, Villanueva Álvarez-Santullano CA, Suárez Fernández R, Pulido Pérez A. Atrofia e hipopigmentación lineal cutánea por inyección intraarticular de corticosteroide. Reumatol Clin. 2019;15:e72–e73.