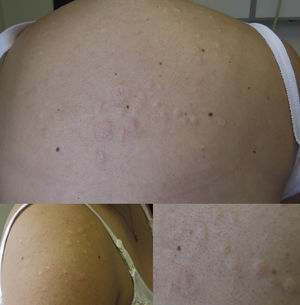
The patient was a 25-year-old woman who had no history of morbid conditions. She presented with lesions on her back, anterior chest and shoulders; at onset, they were painful but became asymptomatic. Physical examination of the regions mentioned above revealed the presence of papules and plaques the color of the skin, which appeared to be lax, that were soft on palpation (Fig. 1). The findings suggested primary anetoderma (PA) and a biopsy of the lesions were performed. The report was as follows: skin with intact epidermis, without atrophy; papillary dermis with no significant changes, whereas in reticular dermis there were focal periadnexal and perifollicular, superficial perivascular lymphoplasmacytic infiltrates. The collagen fibers were somewhat disorganized from the mid-reticular dermis to the deep dermis, and sclerosis was not observed with van Gieson staining. Verhoeff's stain revealed a marked reduction of elastic fibers in regions of the mid-reticular and deep dermis. There was no increase in dermal mucin or changes in the basement membrane. These results led to a diagnosis of PA; although the specimens presented signs of inflammatory dermatosis, these were nonspecific findings and did not enable us to determine the cause of the dermatitis that produced the anetoderma.
The patient subsequently discontinued follow-up monitoring, and 6 years later she had a fetal loss. Thus, given the suspicion that there might be an underlying immunological disorder, she underwent a complete study that confirmed the diagnosis of systemic lupus erythematosus and antiphospholipid syndrome. At the present time, the patient is being treated for her diseases, with no secondary complications.
Primary anetoderma is an uncommon disorder that occurs on previously healthy skin, where there is a localized partial or total loss of the elastic fibers in the papillary and/or mid-reticular dermis, provoking a focal flaccidity of the skin.1 The clinical signs are papules or normochromic or pink plaques, measuring from 0.5 to 3cm in diameter, with areas of atrophy and secondary soft herniation (Fig. 1).2 At the present time there is growing evidence with respect to the association between PA and certain autoimmune disorders; the most widespread of the latter is the presence of antiphospholipid antibodies, whether as an isolated laboratory finding, as part of antiphospholipid syndrome or together with other signs (clinical and/or from laboratory tests) of autoimmunity, including systemic lupus erythematosus.3 These immunological diseases may develop many years after the onset of PA. For this reason, any patient who has been diagnosed with PA should undergo clinical and laboratory follow-up in the search of autoimmune disorders.
Ethical DisclosuresProtection of human and animal subjectsThe authors declare that no experiments were performed on humans or animals for this study.
Confidentiality of dataThe authors declare that no patient data appear in this article.
Right to privacy and informed consentThe authors have obtained the written informed consent of the patients or subjects mentioned in the article. The corresponding author is in possession of this document.
Conflict of InterestsThe authors declare that they have no conflict of interests.
Please cite this article as: Hasbún Acuña P, Cullen Aravena R, Queirolo González A, Corredoira Salum Y. Anetodermia primaria: un predictor cutáneo de autoinmunidad. Reumatol Clin. 2018;14:242–243.