To assess the relationship between the increase of faecal calprotectin, anti-Saccharomyces cerevisiae antibodies (ASCA) and disease markers in a group of patients with spondyloarthritis.
MethodsWe evaluated patients who were at least 18 years old and met the Assessment in Spondyloarthritis International Society (ASAS) criteria for spondyloarthritis or the New York modified criteria. We analysed activity criteria, physical function, analytical criteria (human leucocyte antigen [HLA] B27, faecal calprotectin, presence of ASCA, among others) and demographic data.
ResultsWe included 33 patients. All but one patient had normal ASCA values. We found statistical significance in the correlation of calprotectin with C-reactive protein (CRP) but not with other parameters. We also found a relationship between calprotectin levels and nonsteroidal anti-inflammatory drug (NSAID) intake (P=.001). We found no relationship between CRP levels and NSAID use. After discontinuation of NSAIDs for one month, we found no significant differences in calprotectin levels (P=.9).
ConclusionFaecal calprotectin is elevated in patients with spondyloarthritis and correlates positively with CRP. Level of faecal calprotectin is not altered by NSAID use. The amount of ASCA present does not change and does not correlate with any clinical parameters in the study population.
Valorar la relación entre la calprotectina fecal, ASCA y marcadores de enfermedad en espondiloartritis (Spa).
MétodosSe evaluaron pacientes≥18 años que cumplían criterios ASAS o criterios modificados de Nueva York. Se analizan criterios de actividad, función física, analíticos y datos demográficos.
ResultadosSe incluyeron 33 pacientes. Todos excepto uno tenían valores normales de ASCA. Encontramos correlación significativa entre calprotectina y PCR pero no con otros parámetros, ni entre los niveles de calprotectina y la toma de AINE (p=0,001). Tampoco entre los niveles de PCR y el uso de AINE. Después de retirar los AINE no encontramos diferencias en los niveles de calprotectina (p=0,9).
ConclusiónLa calprotectina fecal está elevada en pacientes con Spa y se correlaciona positivamente con la PCR. La elevación de la calprotectina fecal no se ve alterada por el uso de AINE. La cantidad de ASCA no cambia y no se correlaciona con ningún parámetro clínico en el estudio poblacional.
Ankylosing spondylitis (AS) is a chronic inflammatory disease that may be associated with extra-skeletal manifestations such as inflammatory intestinal disease (IID), among others. There is a high incidence of IID in patients with AS. There is even a theory that AS and Crohn's disease share the same etiopathogenesis.1 25%–50% of AS patients without IID symptoms have an intestinal histology with inflammation, according to some works.1
Increased intestinal permeability has been found in IID as well as in AS, shown by the presence of certain markers such as anti-Saccharomyces cerevisiae antibodies (ASCA) and calprotectin, among others.1,2
Faecal and serum calprotectin is used to differentiate between IID and functional intestinal disease.3,4 A rise in serum calprotectin has been observed in patients with spondyloarthritis (Spa), with a good correlation with other markets (PCR and VSG, among others), disease progression2 with response to treatment.3,5
There are doubts as to whether the concentration of faecal calprotectin in AS patients is linked to taking non-steroid anti-inflammatory drugs (NSAID). In some series patients with AS who do not take NSAID have similar concentrations of calprotectin to patients with IID.4
In other diseases, such as rheumatoid arthritis and psoriatic arthropathy, faecal calprotectin may act as an independent predictor of joint injury,4,6 and it is associated with vascular alterations.7
ObjectivesTo discover whether the rise in faecal calprotectin and ASCA is associated with activity and physical function markers in patients with Spa.
We will also analyse the association of calprotectin and ASCA with taking NSAID and with other relevant parameters (HLA-B27 positivity or treatments, among others).
Material and MethodsThe patients, who were over the age of 18 years old, were recruited in the dedicated spondyloarthritis department of the University Hospital Virgen de la Arrixaca, Murcia, sequentially in the order of their visits. Patients diagnosed non-radiographic axial spondyloarthritis were included, according to ASAS criteria, as were those diagnosed AS according to the modified New York criteria.
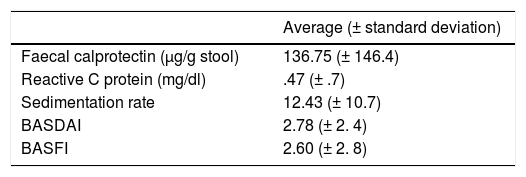
BASDAI and ASDAS-PCR were included as disease activity variables, together with others for physical functioning (BASFI) and to evaluate the disease. Analytical variables were included, such as sedimentation velocity, reactive C protein, the presence of HLA-B27, blood levels of ASCA and faecal calprotectin levels (microgram/gram). ELISA technique was used to detect faecal calprotectin, and 50μg/g stool was considered to be the upper limit of normality.
Patients under the age of 18 years old were excluded, as were those who found it difficult to fill out the questionnaires and those without a definitive diagnosis and/or with another type of spondyloarthritis, including psoriatic arthropathy.
A descriptive analysis was carried out, together with a correlation study and comparison of averages for non-parametric variables (SPSS 15.0). We performed a lineal regression analysis to evaluate the predictive capacity of the variables regarding faecal calprotectin levels.
ResultsThirty-three patients were included (22 men). 54.8% were AS and the others were cases of non-radiographic axial spondyloarthritis.
The average age was 46.5 (±13.6) years old, and 80% of the patients were HLA B27 positive.
51.5% of the patients took an NSAID every day. 39.4% were only taking NSAID, while 6% were taking non-biological immunosupressors, 30.3% were taking biological anti-TNF alpha drugs and 21.2% were untreated.
Table 1 shows the other characteristics of the patients.
All of the patients except one had normal ASCA levels.
84.4% of the patients had levels≥50μg/g of faecal calprotectin, and 47% had levels≥100μg/g.
We found no differences in levels of faecal calprotectin according to the diagnosis (P=.43). This was also the case with the activity parameters, including acute phase reagents (PCR and VSG).
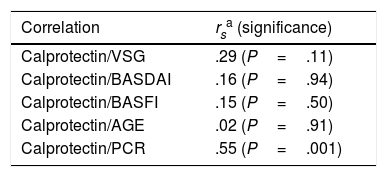
The faecal calprotectin level was only statistically correlated with PCR (P=.001; rs=.55) (Table 2).
Correlation Between Calprotectin and BASDAI, BASFI, Age and PCR.
| Correlation | rsa (significance) |
|---|---|
| Calprotectin/VSG | .29 (P=.11) |
| Calprotectin/BASDAI | .16 (P=.94) |
| Calprotectin/BASFI | .15 (P=.50) |
| Calprotectin/AGE | .02 (P=.91) |
| Calprotectin/PCR | .55 (P=.001) |
No relationship was found between calprotectin levels and the diagnosis or HLA B27 positivity.
We found no association between PCR levels and NSAID administration (P>.05).
The lineal regression study included the level of calprotectin as a dependent variable, and the predictive variables were the BASDAI, PCR, VSG, sex, age and diagnosis. We obtained a corrected R2 determination coefficient=.04, and none of the variables were statistically significant.
We wanted to see whether the increase in calprotectin could be secondary to NSAID administration. For this purpose, a subgroup of 13 patients (8 men) who were taking a NSAID and had a high level of calprotectin>50μg/g were subjected to a second determination of calprotectin as well as the other variables, after one month without taking a NSAID:
- •
Their average age was 47 years old (±10.25).
- •
No significant differences were detected between the levels of acute phase reagents, BASDAI, BASFI and the overall evaluation of the patient (EVA), before and after the withdrawal of the NSAID.
- •
After the withdrawal of the NSAID we found no significant differences in the average levels of calprotectin (92 vs 110, P=.9) or in the other parameters.
- •
We found no differences in the percentage of patients with calprotectin>50μg/g before and after.
- •
Nine patients were assessed by a digestive system specialist using colonoscopy. One patient was diagnosed with irritable bowel syndrome and probable enteropathy caused by a NSAID.
In rheumatology, several studies associate disease activity in patients with Spa with microscopic inflammatory digestive pathology.
In this work we found a positive correlation between faecal calprotectin and PCR in our spondyloarthritis series. The association with other inflammation or activity markers was not confirmed.
Practically 100% of the patients had normal levels of ASCA, so that it can be deduced that this marker would not be useful as an activity indicator.
Raised calprotectin level has been associated in some spondyloarthritis patient cohorts with NSAID administration. In this work we analysed calprotectin levels following NSAID withdrawal in a subgroup of patients, and we found that there was no significant change in the said levels. Nor were alterations found in the colonoscopy of these patients. Disease activity may be a reason for the association between calprotectin and NSAID administration: patients with inflammation and pain take NSAID to control it. The lack of a relationship between treatment with a NSAID and PCR may be due to the rarity of this marker rising in disease of this type.
The small number of patients in this study should be taken into account as a source of distortion. This may be the reason why there is a lack of correlation between calprotectin and other activity parameters such as the BASDAI.
Another distortion that we can analyse is the time without NSAID administration in the 13-patient subgroup. According to some other studies,1 some calprotectin analysis tests recommend not taking NSAID during the two days prior to taking the sample. A recent study8 which analyses the possible influence of NSAIDs on levels of faecal calprotectin, suggests that two weeks without NSAID are sufficient for levels of faecal calprotectin to be unaltered by these drugs.
Conclusions- •
Faecal calprotectin levels are raised in patients with spondyloarthritis, correlating positively with PCR.
- •
Raised levels of faecal calprotectin are not modified by taking an NSAID or not.
- •
ASCA levels in blood neither vary nor show any relationship with clinical parameters in the population studied.
The authors have no conflict of interests to declare.
Please cite this article as: Moreno Martínez MJ, Moreno Ramos MJ, Linares Ferrando LF. Relación de calprotectina fecal y anticuerpos antisacaromices con otros marcadores de actividad en pacientes con espondiloartritis. Reumatol Clin. 2019;15:360–362.