We present the case of a 56-year-old male patient, allergic to penicillin, with a history of hypercholesterolaemia, diabetes mellitus and seropositive, nodular, and erosive rheumatoid arthritis, diagnosed in 2009. He had received several biological treatments (etanercept, adalimumab, tocilizumab, rituximab, abatacept, which were withdrawn due to inefficacy or adverse effects) and was currently being treated with 25mg methotrexate weekly, 5mg of celecoxib and tofacitinib every 12h, without incident and with the rheumatic disease in remission.
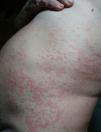
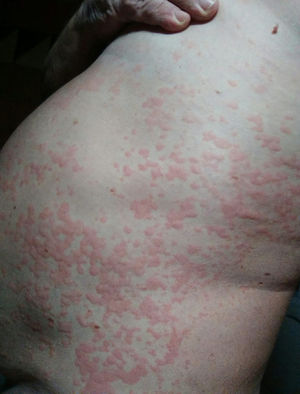
He presented at the emergency department on 3 occasions due to the presentation of a generalized, very itchy, wheal-like rash of more than 24h onset, which left hyperpigmentation and on occasions purpura where the wheals were located (Fig. 1). The rash was accompanied by a general feeling of malaise, a tightening of the chest, glottic and uvula labial edema. The patient was administered with intravenous glucocorticoids and antihistamines in the emergency department, with rapid improvement of symptoms. During one visit adrenaline was required. Despite the treatment with high doses of systemic glucocorticoids, maximum doses of second-generation antihistamines, sedating antihistamines and ranitidine, the patient continued having extremely itchy general lesions.
Analysis revealed high acute phase reactants, leucocytosis with neutrophilia, d-dimer of 1080ng/ml, normal complement, negative antinuclear antibodies and IgE 383KU/l with specific IgE negative to Anisakis and Ascaris. A punch skin biopsy was performed on an acute lesion which showed mild neutrophilic vasculitis in the superficial and deep dermis with an absence of eosinophils, compatible with urticarial vasculitis (UV). Computerized tomography of the chest was performed, together with an echocardiogram, which were both normal.
- •
Once the diagnosis of normocomplementemic UV (NUV) had been established we considered whether the cutaneous symptoms were toxicoderma from the new immunosuppressants (Janus kinase inhibitor) or some other autoimmune process associated with the patient's rheumatoid arthritis. We ruled out the first option because the patient had been treated with tofacitinib for months without complications and because although the treatment was temporarily suspended, the skin lesions persisted. Symptoms were not controlled, and we therefore considered treatment with omalizumab. Other therapeutic options were ruled out (colchicine, sulphone or cyclosporine) due to the patient's immunosuppression. Several published cases have reported on the use of omalizumab in UV1–5 aside from specification sheet usage. The article by De Brito et al.3 reviewed cases published until 2018 in patients with UV and comparing the efficacy of omalizumab, observed that the NUV responded better to omalizumab than the hypocomplementemics (HUV). This led them to believe that there could be 2 diseases with different physio pathological mechanisms. In NUV the IgE and mastocytary cells would play a more important role whilst the endothelial damage from immunocomplex deposits would be more involved in the HUV, which would therefore not respond so well to omalizumab.
The case was presented and approved by the committee of special hospital uses and the patient signed an informed consent form. Treatment was initiated with omalizumab at a dose of 300mg/every 4 weeks, maintaining the antihistamines for several weeks and withdrawing the glucocorticoids. The skin lesions disappeared after the first administration of therapy. The patient has to date received 6 cycles of omalizumab at a dose of 300mg/every 4 weeks and continues to be asymptomatic.
Both the acute phase reactants and the d-dimer reached normal levels. It was possible to withdraw the glucocorticoids maintaining just 5mg/day (arthritis control). Treatment with tofacitinib was re-started 2 weeks after treatment with omalizumab, without incident. On re-initiation of methotrexate the patient presented with an episode of transaminitis which was resolved on dose reduction. No interactions or infections occurred during combined treatment.
This is the first case to be described in the literature of a patient with rheumatoid arthritis and NUV, both autoimmune diseases with difficult management. The patient presented with an extremely rapid and effective response to omalizumab with total disappearance of the skin lesions.
Please cite this article as: Baliu-Piqué C, Narvaez-Garcia FJ, Retamero A, Grados D. Dos enfermedades autoinmunes de difícil manejo. Reumatol Clin. 2021;17:427–428.